How to Prevent Skin Rashes: Hygiene, Lifestyle, and Medical Prevention Strategies
Prevention is the most powerful tool in skin health. While treating an active rash requires time, prescription medications, and often significant discomfort, the underlying conditions that produce most rashes — compromised skin barriers, allergen sensitization, microbial imbalance, and chronic inflammation — are substantially modifiable through daily habits and targeted lifestyle choices.
Rashes form when the skin's defensive systems are overwhelmed. The skin barrier — a multilayered structure of cells, lipids, and proteins — is the body's primary defense against environmental threats. When this barrier is disrupted by dryness, harsh cleansers, friction, heat, or underlying inflammation, allergens, pathogens, and irritants penetrate more easily, triggering the immune responses that produce redness, itching, swelling, and rash.
Understanding how rashes form reveals exactly where prevention intervenes: strengthen the skin barrier daily, reduce allergen and irritant exposure, control inflammatory triggers (stress, diet, infection), and address specific vulnerabilities for chronic conditions. Each of these intervention points is addressed in depth in this guide.
Whether you are trying to prevent your first rash, reduce the frequency of recurring flares, protect your children's sensitive skin, or manage a chronic skin condition, this guide provides practical, evidence-based strategies organized by category and mechanism of action.
Daily Hygiene Practices That Prevent Rashes
The foundation of rash prevention is a consistent, gentle skin care routine that cleanses effectively without disrupting the natural protective barrier.
Use gentle, fragrance-free cleansers
Standard soaps have an alkaline pH (9–10) that disrupts the skin's naturally acidic pH (4.5–5.5), impairing the barrier. Choose pH-balanced, fragrance-free cleansers — look for 'syndet' (synthetic detergent) bars or gentle liquid cleansers. Brands formulated specifically for sensitive skin (e.g., Dove Sensitive, Vanicream) maintain barrier integrity.
Avoid over-washing
Washing skin more than once daily with soap — unless occupationally required — strips the natural oils (sebum) that form part of the skin's protective film. Over-washing is a significant driver of irritant contact dermatitis, particularly on the hands. Rinse hands with water and use cleanser only when genuinely needed.
Manage sweat proactively
Sweat left on skin, particularly in folds and under athletic clothing, creates a warm, moist environment ideal for fungal and bacterial growth. Shower promptly after exercise, change out of sweaty clothing immediately, and use absorbent powders (non-talcum) in skin folds if you sweat heavily. Antiperspirant applied to affected areas can reduce sweat in fold zones.
Dry skin folds thoroughly
The neck, groin, underarms, beneath breasts, and between toes are the highest-risk locations for intertrigo (skin fold rash) and fungal infection because trapped moisture prevents evaporation. Pat these areas completely dry after bathing — do not rub, which causes friction irritation. A hairdryer on a low, cool setting accelerates drying in difficult-to-reach folds.
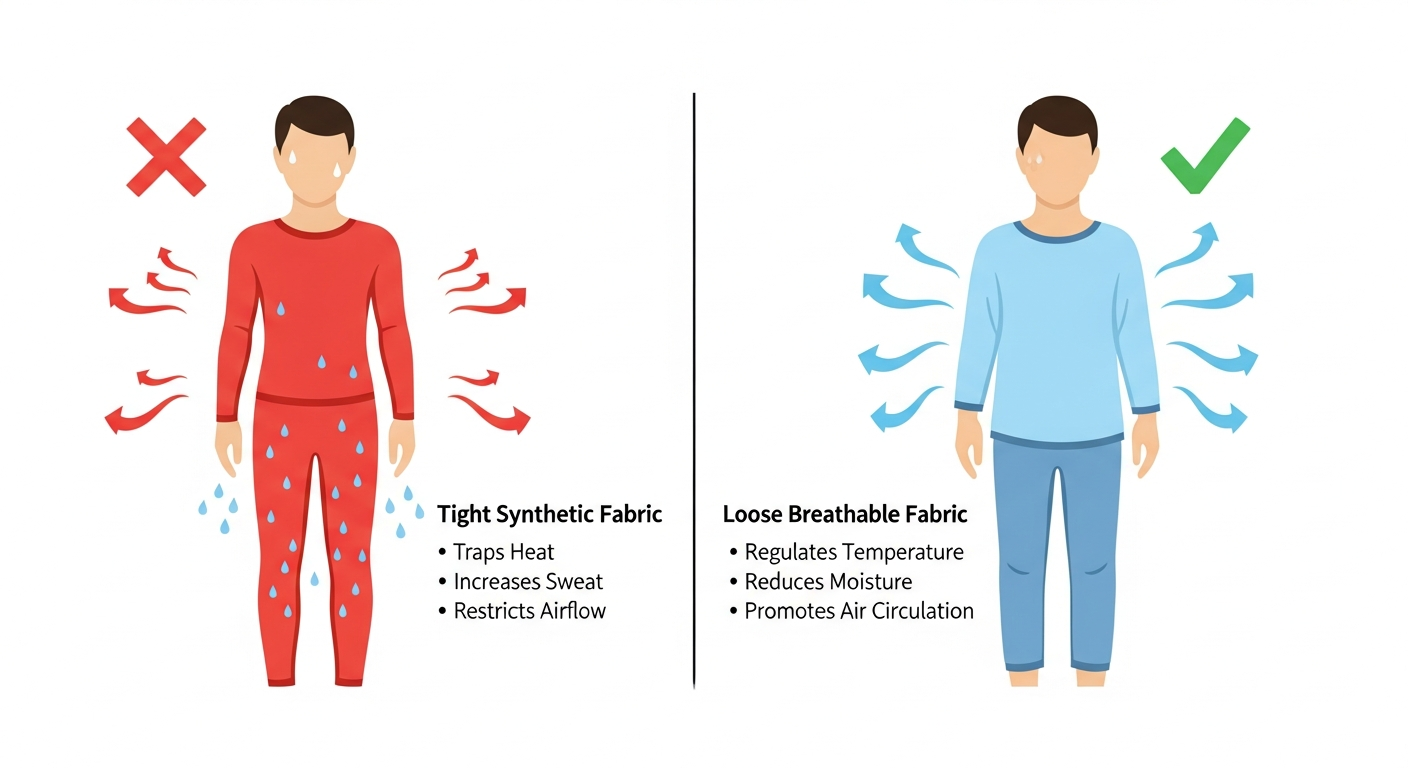
Choose breathable fabrics
Synthetic fabrics (polyester, nylon, spandex) trap heat and moisture against the skin, raising local temperature and humidity significantly above skin-healthy thresholds. Natural fibres — particularly 100% cotton, bamboo, and merino wool — wick moisture away and allow air circulation. Loose-fitting clothing reduces friction, a separate but significant rash trigger.
Moisturize immediately after bathing
The optimal window for moisturizer application is within 3 minutes of towel-drying, when residual skin moisture is still present. This 'soak and seal' method traps hydration in the skin rather than losing it to evaporation. Apply a generous layer of fragrance-free, ceramide-containing cream or ointment from neck to feet daily.
Allergy Prevention Strategies
Allergic contact dermatitis accounts for a significant proportion of chronic rashes. Prevention depends on allergen identification and avoidance.
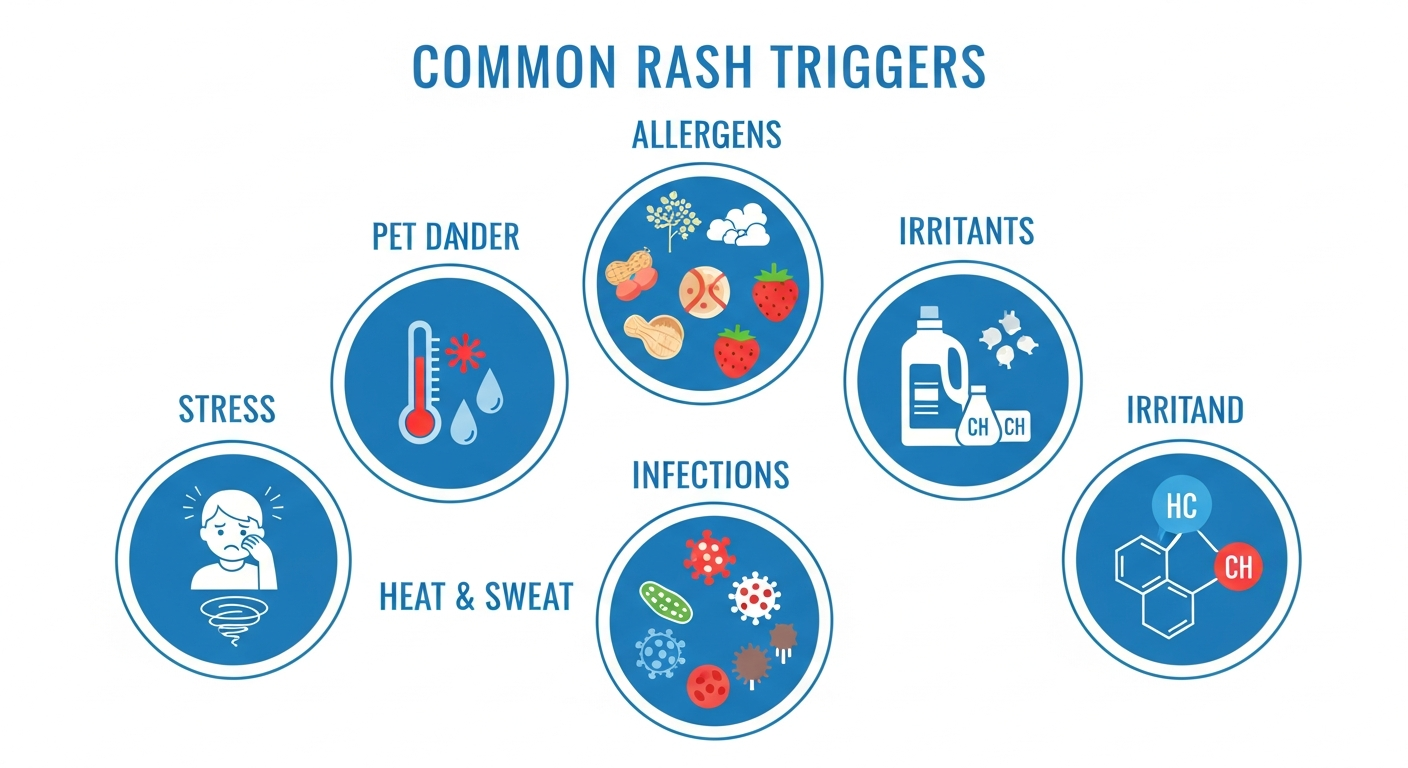
Switch to fragrance-free personal care products
Fragrance is the most common cause of allergic contact dermatitis, accounting for up to 30–45% of positive patch test reactions. This includes perfumes, fragranced moisturizers, shampoos, deodorants, and laundry detergents. 'Unscented' does not mean fragrance-free — masking fragrances are still present. Look specifically for 'fragrance-free' labeling.
Patch test new cosmetics before full use
Before applying a new skin care product to the face, neck, or body, apply a small amount to the inner forearm and leave for 24–48 hours. Monitor for any redness, itching, or swelling. This simple step identifies contact sensitivities before a widespread reaction develops. Allergy to a cosmetic ingredient becomes a permanent sensitization — prevention before first exposure is the goal.
Identify and systematically avoid known irritants
Common irritants beyond fragrance include: nickel (jewelry, belt buckles, jean buttons), latex (gloves, condoms, balloons), preservatives (parabens, methylisothiazolinone in personal care), rubber accelerators (in elastic, gloves, shoes), and acrylates (nail products). If you've had a documented allergic reaction, keep a written list of ingredients to avoid and read every product label.
Use protective gloves for chemical exposure
Occupational chemical exposure is a leading cause of hand dermatitis, affecting hairdressers, healthcare workers, cleaners, mechanics, and food industry workers. Wear appropriate gloves for each exposure: nitrile for most chemicals (latex-allergic safe), PVC for prolonged water work, cotton liners under gloves for extended wear to absorb sweat. Change gloves every 30–60 minutes in extended work sessions.
Get formal patch testing after recurrent reactions
If you experience recurring rashes in consistent locations — particularly the hands, face, or neck — that have not been identified through avoidance trials, formal patch allergy testing by a dermatologist identifies the specific culprit. The European Baseline Series plus extended panels test 30–150 allergens. This is the most accurate method available and permanently guides your avoidance strategy.
Use fragrance-free laundry products
Residual laundry detergent and fabric softener left in fabrics remain in contact with the skin for hours during wear. This is a common but underrecognized source of widespread body rashes, particularly in children and those with eczema. Use fragrance-free, dye-free detergents and run an extra rinse cycle. Fabric softeners are unnecessary and add allergen risk — omit them.
Heat and Sweat Rash Prevention
Heat rash (miliaria) and sweat-related skin conditions are among the most preventable rashes through environmental and clothing strategies.

Hydrate adequately — especially in heat
Adequate hydration maintains normal sweating efficiency. Dehydration leads to concentrated sweat with higher salt content, which is more irritating to the skin surface and more likely to trigger miliaria. Aim for 2–3 litres of water daily in warm climates or during physical activity, increasing fluid intake before outdoor exertion.
Wear loose, light, moisture-wicking clothing
Tight clothing increases skin-to-skin and fabric-to-skin friction and traps sweat against the surface. Choose loose-fitting, light-coloured garments in natural fibres or performance moisture-wicking fabrics designed for athletic use. Avoid nylon and polyester next to skin in hot environments. Change promptly when clothing becomes saturated with sweat.
Use cooling strategies proactively
Cooling fans, air conditioning, cool wet towels, and cool (not cold) water immersion reduce sweating intensity and skin temperature. In outdoor settings, seek shade during peak heat hours (10am–4pm). Cold packs applied to pulse points (wrists, neck, groin) rapidly reduce core temperature. For athletes, cool water misting during exercise significantly reduces heat rash incidence.
Reduce workplace heat exposure
Workers in kitchens, foundries, outdoor construction, and other hot environments have significantly higher heat rash rates. Workplace strategies include scheduled cool breaks, cooling stations, personal cooling vests, and scheduling the most physically demanding tasks for cooler morning hours. Employers in high-temperature environments are increasingly required to provide heat stress management protocols.
Infection Prevention
Infectious rashes — bacterial, fungal, and parasitic — are highly preventable with targeted hygiene and exposure management.
Prevent fungal infections with dry skin practices
Dermatophyte fungi (ringworm, athlete's foot, jock itch) thrive in warm, moist environments. Prevention: dry thoroughly between toes and in skin folds after bathing, wear moisture-wicking socks and breathable shoes, change socks daily, use antifungal powder in shoes if you are susceptible, and avoid barefoot contact with pool surrounds, gym floors, and locker rooms.
Prevent bacterial skin infections
Staphylococcus and Streptococcus bacteria cause impetigo, folliculitis, and cellulitis, often entering through small skin breaks. Prevention: keep cuts and abrasions clean and covered, avoid picking at skin, treat eczema promptly to prevent skin barrier breaks, ensure swimming pool and hot tub hygiene, and avoid sharing personal items (towels, razors) with others.
Prevent parasitic infestations
Scabies and lice spread through direct skin contact or shared bedding and clothing. Prevention: avoid close physical contact with diagnosed individuals until treatment is complete, do not share bedding, clothing, or towels, wash bedding and clothing at 60°C during outbreaks, and treat all household contacts simultaneously if infestation is confirmed to prevent re-infection cycles.
Gym and locker room hygiene
Shared gym equipment, mats, and changing facilities are significant transmission vectors for fungal infections (tinea), staphylococcal skin infections, and molluscum contagiosum. Strategies: always wear footwear in communal showers and around pools, use a clean towel barrier between your skin and shared equipment, shower promptly after gym use, and do not share towels, clothing, or footwear.
Diet and Immune Health
Nutritional status directly influences skin barrier function, inflammatory response, and immune regulation — all of which affect rash susceptibility.
Follow an anti-inflammatory diet
A diet high in ultra-processed foods, refined carbohydrates, and industrial seed oils promotes systemic inflammation via elevated IL-6, TNF-α, and prostaglandin E2 — the same inflammatory pathways that drive eczema and psoriasis flares. Mediterranean diet patterns (abundant vegetables, olive oil, oily fish, legumes, whole grains) have the strongest evidence base for reducing inflammatory skin disease burden.
Stay well hydrated
Chronic mild dehydration impairs skin barrier function by reducing intercellular lipid content and transepidermal water loss regulation. Even a 2% reduction in body water reduces skin elasticity and barrier efficiency measurably. While drinking water alone cannot cure dry skin, adequate hydration (2–3L/day) supports optimal barrier physiology alongside topical moisturizing.
Consider key vitamin and mineral status
Deficiencies in vitamin D (affects immune regulation and skin barrier gene expression), vitamin E (antioxidant protection), zinc (wound healing and immune function), and omega-3 fatty acids (anti-inflammatory eicosanoids) are each associated with increased inflammatory skin disease severity. A balanced diet typically meets these needs; supplementation should be guided by testing rather than routine supplementation without deficiency evidence.
Understand the gut-skin connection
The gut microbiome influences skin inflammation through the gut-skin axis — a bidirectional communication pathway involving immune cells, inflammatory mediators, and shared microbial metabolites. Dysbiosis (gut microbiome imbalance) is increasingly associated with eczema, psoriasis, and rosacea. Probiotic supplementation and dietary fibre intake (supporting beneficial bacterial growth) show modest but emerging evidence for reducing eczema severity, particularly in infants.
Stress and Rash Flare Prevention
Psychological stress is one of the most powerful and consistent triggers of inflammatory skin flares — and one of the most actionable prevention targets.
How Stress Hormones Affect Skin
Acute stress triggers cortisol and adrenaline release, while chronic stress sustains elevated baseline cortisol. Cortisol suppresses barrier repair gene expression (reduced filaggrin and ceramide production), impairs wound healing, and triggers mast cell degranulation — releasing histamine that drives itch. Neuropeptides released during stress (substance P, nerve growth factor) directly stimulate skin immune cells, amplifying inflammatory cascades in eczema, psoriasis, and rosacea.
Sleep Quality and Skin Repair
The skin undergoes its primary repair and regeneration during deep sleep (NREM stages 3–4), when blood flow to the skin increases and growth hormone pulses promote cellular renewal and barrier repair. Chronic sleep deprivation of even 1–2 hours per night measurably increases transepidermal water loss (barrier dysfunction) and raises systemic inflammatory markers. Prioritizing 7–9 hours of quality sleep is a concrete, evidence-based skin health intervention.
Evidence-Based Relaxation Methods
Mindfulness-based stress reduction (MBSR) programs show significant reduction in psoriasis and eczema severity scores in randomized controlled trials. Cognitive behavioral therapy (CBT) for itch management reduces scratching behavior and secondary skin damage. Daily moderate aerobic exercise (150 minutes/week) reduces systemic inflammation via anti-inflammatory myokines. Diaphragmatic breathing activates the parasympathetic nervous system within minutes, reducing cortisol and histamine release.
Preventing Chronic Rash Conditions
Chronic skin conditions require ongoing maintenance strategies — not just reactive treatment of active flares.
| Condition | Key Triggers | Prevention Strategy | Maintenance Products |
|---|---|---|---|
| Eczema | Dry skin, irritants, sweat, stress, allergens | Daily moisturizing, fragrance-free products, identify food/contact triggers, manage stress | Ceramide-based emollients, wet wrap therapy during flares |
| Psoriasis | Stress, strep infections, alcohol, NSAIDs, skin trauma | Stress management, avoid smoking and excess alcohol, treat infections promptly, gentle skin care | Coal tar shampoo, vitamin D analogue creams, biologics for severe cases |
| Contact Dermatitis | Specific allergens (nickel, fragrances, rubber), irritants (detergents, chemicals) | Patch testing to identify allergens, allergen avoidance, protective gloves, barrier creams | Barrier cream, hypoallergenic substitutes for identified allergens |
| Fungal (Tinea) | Moisture, warmth, shared surfaces, skin barrier breaks | Keep skin dry, change socks daily, use antifungal powder in prone areas, avoid barefoot in public | Prophylactic antifungal powder, moisture-wicking socks, breathable footwear |
Children's Rash Prevention Tips
Children's skin is thinner, has a less mature barrier, and mounts immune responses differently — requiring age-specific prevention strategies.
Change nappies frequently with barrier cream
Diaper dermatitis affects up to 35% of infants at any given time. The combination of prolonged moisture, friction, and ammonia from urine creates ideal conditions for skin breakdown and secondary Candida infection. Change nappies every 2–3 hours (more frequently for newborns), cleanse with fragrance-free wipes or water, dry thoroughly, and apply a thick zinc oxide barrier cream at every change.
Use only paediatric-formulated skin products
Adult skin care products — even 'natural' ones — often contain concentrations of fragrances, preservatives, and active ingredients unsuitable for infant skin. Use products specifically formulated and tested for paediatric use, with minimal ingredient lists. For infants under 6 months, plain emollient (petroleum jelly or fragrance-free aqueous cream) is safest for moisturizing.
Prevent school transmission of infectious rashes
Impetigo, ringworm, molluscum contagiosum, and hand-foot-and-mouth disease spread readily in school and nursery settings. Teach children not to share towels, clothing, or sports equipment. Treat any infectious rash promptly and follow school exclusion guidelines (typically until lesions are crusted/healed for impetigo; no exclusion needed for molluscum or most viral rashes).
Dress children for weather and activity
Overdressing infants is a significant cause of heat rash in the first months of life, when temperature regulation is immature. The 'one layer more than an adult' guideline is appropriate, but avoid bulky synthetic fabrics in warm conditions. For outdoor play, dress children in sun-protective fabrics and apply broad-spectrum SPF 30+ sunscreen (for children over 6 months) to exposed areas.
Emollient therapy for atopic infants
There is growing evidence that early, proactive emollient therapy in infants with a family history of atopy (eczema, asthma, hay fever) can delay or reduce the development of eczema by strengthening the skin barrier during its maturation period. Start daily full-body emollient application from the first weeks of life in high-risk infants, using fragrance-free, preservative-minimal products.
Identify food triggers early in eczematous children
In approximately 30–40% of children with moderate-to-severe eczema, specific food allergens (egg, cow's milk, peanut, wheat, soy) exacerbate skin symptoms. Identification requires structured elimination and reintroduction trials under medical supervision — not self-administered elimination diets, which risk nutritional deficiency. Early introduction (not avoidance) of allergenic foods from 4–6 months is now recommended to reduce sensitization risk.
Outdoor Rash Prevention
Outdoor environments introduce unique rash risks from insects, plants, sun, and water that require specific protective strategies.
Insect Protection
- Apply DEET (20–30%) or picaridin insect repellent to exposed skin in tick and mosquito habitats
- Wear long-sleeved, light-coloured clothing in woodland and grassland areas
- Check for and remove ticks within 24 hours — this reduces Lyme disease transmission risk significantly
- Apply permethrin to clothing and gear (not skin) for extended outdoor exposure
- Seek medical attention promptly for bull's-eye rash (erythema migrans) — Lyme disease treatment is most effective early
Plant Exposure Awareness
- Learn to identify poison ivy, poison oak, and poison sumac in your region — 'leaves of three, let it be'
- Cover skin fully when working in areas where allergenic plants are present
- Wash all exposed skin within 30 minutes of potential contact — urushiol oil remains active for hours
- Wash gardening gloves, tools, and clothing separately after possible plant contact
- Pre-treat with barrier creams (IvyBlock) before entering high-risk plant environments
Sunscreen Strategies
- Apply broad-spectrum SPF 30–50 sunscreen 20 minutes before sun exposure, reapply every 2 hours
- Choose mineral sunscreens (zinc oxide, titanium dioxide) for sensitive skin — less likely to cause contact allergy
- Chemical sunscreen ingredients (oxybenzone, avobenzone) can trigger photoallergic reactions in some individuals
- Cover with UPF 50+ clothing and wide-brimmed hat — physical protection is more reliable than sunscreen alone
- Avoid sun between 10am–4pm, when UV intensity is highest, particularly if on photosensitising medications
Frequently Asked Questions
Evidence-based answers to the most common rash prevention questions.
Learn More About Rash Symptoms and Diagnosis
Medical Disclaimer: The prevention strategies, product recommendations, and nutritional information on this page are for general educational purposes only and do not constitute medical advice. Individual responses to prevention strategies vary, and underlying conditions may require professional evaluation and treatment. Always consult a qualified dermatologist or healthcare provider before changing your skin care routine or starting new supplements, particularly if you have a diagnosed skin condition. Read our full medical disclaimer.