Itchy Red Rash: Causes, Diagnosis, and Treatment
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
March 5, 2026
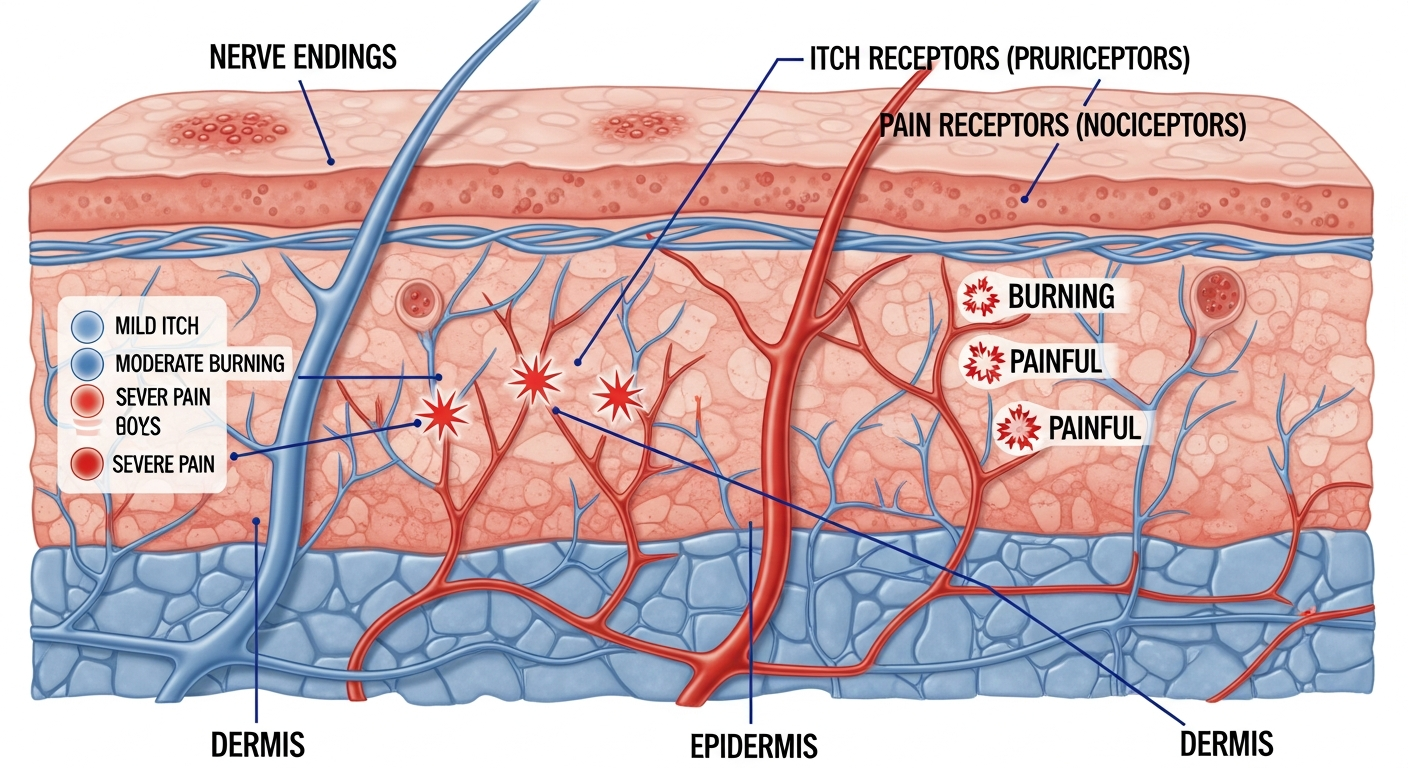
An itchy red rash is the single most common presentation in dermatology — and one of the most diagnostically variable. Dozens of conditions produce this symptom combination, ranging from the completely benign (contact dermatitis from a new fabric softener) to conditions that require urgent evaluation (severe allergic reaction, bullous pemphigoid). The critical diagnostic work in evaluating an itchy red rash comes from five additional questions: Where is it? (Location is the most important diagnostic clue — inner elbows suggest eczema, ring-shaped suggests ringworm, exactly where jewelry sits suggests nickel allergy.) How did it start and how quickly? (Hives appear within 30 minutes; contact dermatitis takes 24–72 hours; eczema flares over days.) Is there blistering? (Blistering itchy rash has a narrower differential — allergic contact dermatitis, dyshidrotic eczema, herpes, chickenpox.) Does it move or stay in one place? (Urticaria migrates within 24 hours; eczema stays in consistent locations.) What are the triggers? (Heat, exercise, and stress point toward urticaria; cosmetic changes toward contact dermatitis.) This guide ranks the most likely causes of itchy red rash by frequency, explains how to narrow down the diagnosis, and describes when the condition becomes serious.
Quick Medical Summary
Possible Causes Ranked: Most to Least Likely
Atopic eczema (atopic dermatitis) is the most common cause of chronic itchy red rash. It affects 15–20% of children and 3–5% of adults globally, is strongly associated with a personal or family history of asthma and hay fever (the atopic triad), and has characteristic locations: inner elbow creases, behind the knees, wrists, neck, and around the eyes. The itch is intense — often worse at night — and the rash is chronic, relapsing, and associated with dry skin. Allergic contact dermatitis is the second most important cause: it requires prior sensitization to an allergen and then produces an intense, blistering, itchy rash in the exact shape and location of allergen contact. The most common allergens globally are nickel (from jewelry and belt buckles), fragrances and preservatives in cosmetics, rubber accelerators in gloves, and poison ivy/oak. The 24–72 hour delay between contact and reaction is a key feature. Urticaria (hives) — rapidly appearing, intensely itchy, raised wheals (welts) that blanch with pressure and migrate within 24 hours — is the third major cause. It results from mast cell degranulation releasing histamine, which causes local skin swelling and itch. Triggers include foods, medications, latex, exercise, cold, and in many cases no identifiable trigger (chronic spontaneous urticaria). Ringworm (tinea corporis) — a dermatophyte fungal infection producing the classic expanding ring with a scaly raised outer border, central clearing, and mild-to-moderate itch — is extremely common and frequently misdiagnosed as eczema or psoriasis. Key diagnostic clue: it expands progressively outward with a distinct active ring border. Polymorphic light eruption (PLE) — itchy papules and vesicles appearing on sun-exposed areas (outer forearms, décolletage, neck) within 1–2 days of sun exposure in spring — affects 10–20% of adults, particularly fair-skinned women.
How to Narrow Down the Diagnosis
The following systematic approach substantially narrows the differential diagnosis of itchy red rash before medical evaluation. Step 1 — Location analysis: Symmetric rash in body fold creases (inner elbows, behind knees) → atopic eczema. Rash exactly where jewelry, watch, or cosmetic product contacts → contact dermatitis (nickel, fragrance). Expanding ring shape on trunk, arm, or leg → ringworm. Widespread, migrating wheals resolving within 24 hours → urticaria. Rash only on sun-exposed areas → PLE or photocontact dermatitis. One-sided band with burning pain → shingles (not primarily itchy — burning pain is more characteristic). Step 2 — Timeline: Appeared within 30 minutes of exposure → urticaria (IgE-mediated). Appeared 24–72 hours after allergen exposure → allergic contact dermatitis. Chronic, relapsing for months or years in same locations → eczema or psoriasis. Appeared after 1–2 weeks of starting a new medication → drug eruption. Step 3 — The blanching test: Apply glass firmly to the rash. Blanching (turns white) → inflammatory rash (urticaria, eczema, contact dermatitis — not urgent). Non-blanching (stays red/purple) → petechiae, purpura, or vasculitis — urgent medical evaluation. Step 4 — Recent changes: New soap, detergent, cosmetic, jewellery, or clothing → contact dermatitis. New medication in last 2 weeks → drug reaction. New pet or outdoors exposure → ringworm, or flea bites. Spring/summer sun exposure → PLE. Step 5 — Associated symptoms: Fever → viral rash or drug reaction rather than simple eczema. Joint swelling → psoriatic arthritis, reactive arthritis, or lupus. Throat tightening → anaphylaxis, use epinephrine and call emergency services.
When the Itchy Red Rash Becomes Serious
The vast majority of itchy red rashes are uncomfortable but not dangerous. However, the following features indicate the rash requires urgent or emergency evaluation. Urticaria (hives) accompanied by throat tightening, facial swelling, breathing difficulty, or dizziness: anaphylaxis — use an epinephrine auto-injector if prescribed and call emergency services immediately. Do not wait to see if symptoms improve. Any rash that does not fade under firm glass pressure (non-blanching): may indicate petechiae, purpura from vasculitis, or meningococcal septicemia. With fever, neck stiffness, or severe headache, call emergency services immediately. Spreading blistering itchy rash with mouth sores, eye redness, or genital blistering, 7–14 days after starting a new medication: Stevens-Johnson Syndrome — stop all suspect medications and go to the emergency department. Intensely itchy rash in web spaces between fingers, on wrists, genitalia, and buttocks, worse at night, affecting multiple household members simultaneously: scabies — requires same-day prescription treatment for all contacts. Widespread itchy red rash developing in pregnancy, particularly affecting the abdomen in the third trimester: PUPPP (pruritic urticarial papules and plaques of pregnancy) — distressing but self-limiting; polymorphic eruption of pregnancy. Any intensely itchy rash in pregnancy with elevated liver enzymes: obstetric cholestasis — requires urgent blood tests, as it raises the risk of stillbirth. Rash persisting despite 4 weeks of appropriate treatment: seek dermatological evaluation to confirm the diagnosis — it may be a condition that mimics eczema but requires different treatment (psoriasis, mycosis fungoides — a rare T-cell lymphoma that presents as a persistent eczema-like rash in adults).
Key Symptoms
- Symmetric itchy rash in elbow/knee creases, dry skin (atopic eczema)
- Intensely itchy rash in exact shape of jewelry or cosmetic contact (contact dermatitis)
- Migrating raised wheals resolving within 24 hours (urticaria)
- Expanding ring with raised scaly border (ringworm)
- Itchy papules on sun-exposed areas after first spring sun (PLE)
- Itchy rash in web spaces with nocturnal itch in multiple contacts (scabies)
- Itchy rash 7–14 days after new medication (drug eruption)
- Hives + throat swelling or breathing difficulty (anaphylaxis — emergency)
Treatment Options
- Eczema: emollient + topical steroid; dupilumab for moderate-severe; trigger avoidance
- Contact dermatitis: identify allergen (patch test); strict avoidance; topical steroid
- Urticaria: cetirizine/loratadine (up to 4× dose); omalizumab for chronic cases
- Ringworm: topical clotrimazole or terbinafine for 4 weeks (full course)
- PLE: SPF 50+ on sun-exposed areas; UVB desensitization for severe cases
- Scabies: permethrin 5% whole body; treat all household contacts same day
- Drug eruption: stop causative drug; antihistamines; monitor for SJS progression
- Anaphylaxis: epinephrine auto-injector + emergency services immediately
| Condition | Location Pattern | Duration of Individual Lesion | Key Distinguishing Feature |
|---|---|---|---|
| Atopic Eczema | Flexural creases, symmetric | Weeks to months (chronic) | Family history of atopy; worse at night |
| Contact Dermatitis | Exactly where allergen contacted | Days to 2 weeks | Matches allergen shape; 24–72h delay |
| Urticaria | Anywhere, migrating | Each wheal <24h | Wheals migrate; blanch with pressure |
| Ringworm | Any, expanding ring | Weeks if untreated | Active scaly ring, central clearing |
| Scabies | Web spaces, wrists, genitalia | Persistent until treated | Night itch; multiple contacts affected |
| Drug Eruption | Trunk spreading outward | Days to 2 weeks after stopping drug | Started with new medication |
Narrow Down Your Diagnosis Further
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.