Why Does My Rash Itch at Night?
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
October 28, 2025
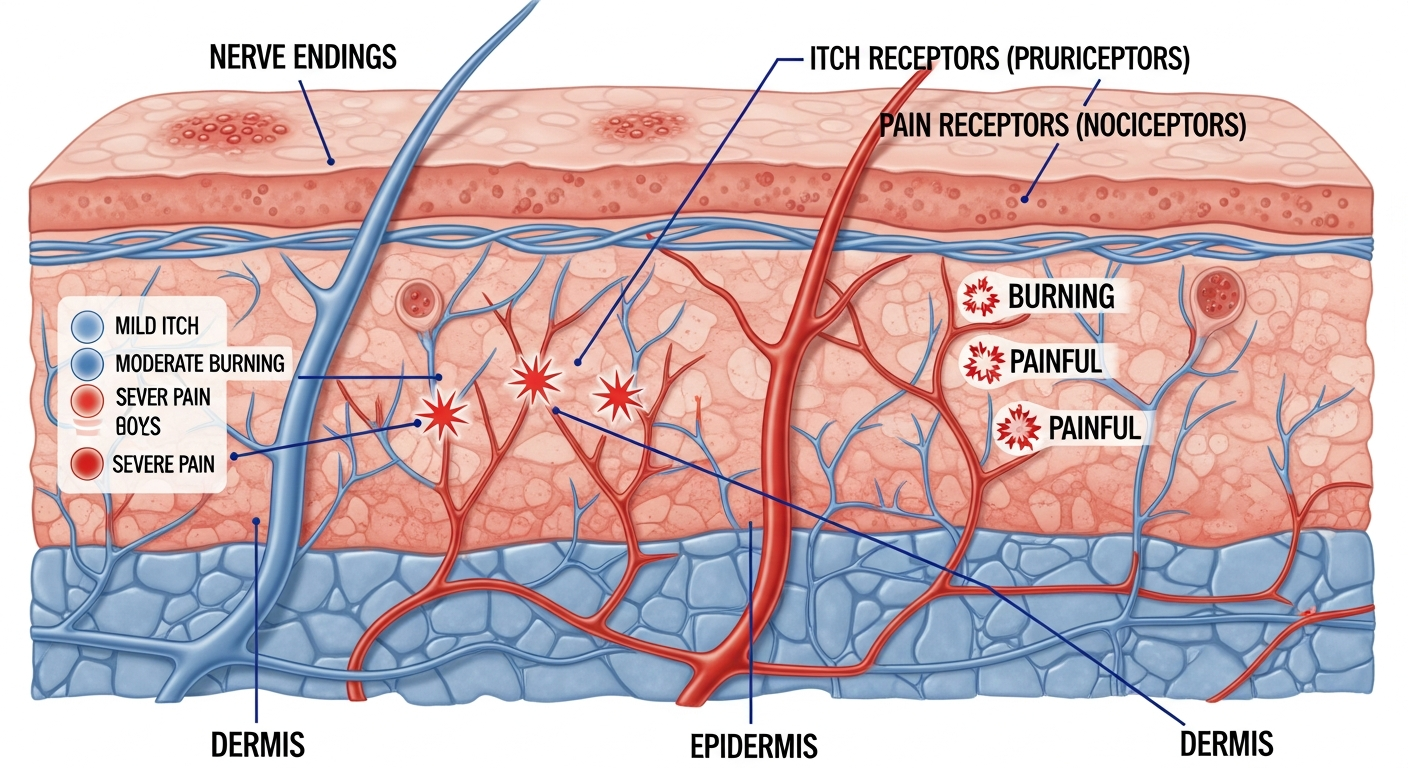
Rashes itch worse at night because of natural changes in your body's circadian rhythm, skin physiology, and environment that all converge after dark. Between 9 PM and 2 AM, your skin loses more water through evaporation (a process called transepidermal water loss), making it drier and more prone to itch. Simultaneously, blood levels of anti-inflammatory cortisol — your body's natural itch suppressant — drop significantly at night, removing the chemical brake on itch signals. Skin temperature also rises in bed, increasing blood flow to the surface, which activates itch receptors. On top of these biological factors, there are fewer daytime distractions to compete with the itch signal at night, making you hyperaware of sensations you barely noticed during the day. Conditions most notorious for severe nocturnal itching include eczema (atopic dermatitis), scabies, psoriasis, cholestasis (liver bile buildup), and chronic kidney disease. Understanding the cause is essential — the treatment for eczema-related night itch is very different from scabies-related night itch.
Quick Medical Summary
The Biology Behind Nighttime Itching
Your skin is regulated by the same 24-hour circadian clock that governs your sleep-wake cycle. During daylight hours, the hypothalamic-pituitary-adrenal axis produces elevated cortisol — a potent anti-inflammatory hormone that damps down the immune activity responsible for itch and inflammation. As evening arrives and cortisol levels decline, this protective suppression lifts. The immune system becomes more active, and inflammatory mediators like histamine, interleukins, and prostaglandins become more concentrated in the skin. This is the primary reason that conditions driven by immune activation — eczema, psoriasis, hives — flare dramatically at night. Simultaneously, your skin's barrier function weakens after dark. The stratum corneum (outermost skin layer) retains less moisture at night, increasing transepidermal water loss, creating dryness, and lowering the itch threshold. Even a slight drop in humidity in a heated or air-conditioned bedroom accelerates this moisture loss. Research published in the Journal of Investigative Dermatology demonstrated that histamine-induced itch peaks between 9 PM and midnight in healthy subjects — meaning even without a skin condition, nighttime is simply the itchiest time of day.
Medical Conditions That Cause Worse Itching at Night
Scabies is perhaps the most characteristic cause of severe nighttime itch. The mite Sarcoptes scabiei is more active when skin is warm, and the host's immune response intensifies at night, producing intense, nearly unbearable itching between the fingers, on the wrists, and across the body after dark. Characteristic burrow lines are a diagnostic clue. Eczema (atopic dermatitis) is the most common cause overall — children especially experience disruptive nighttime itch-scratch cycles that fragment sleep. Psoriasis follows the same circadian pattern, with plaques feeling more inflamed and itchy at night despite looking similar to daytime. Cholestasis — bile salt buildup caused by liver or gallbladder disease, intrahepatic cholestasis of pregnancy, or primary biliary cholangitis — causes severe generalized nighttime itch without a visible rash, a crucial distinguishing feature. Chronic kidney disease (uremia) similarly produces generalized pruritus worse at night. Hodgkin's lymphoma classically causes nocturnal pruritus that may appear months before the diagnosis. If your nighttime itch has no visible rash, or is accompanied by fatigue, jaundice, or unintentional weight loss, seek medical evaluation promptly.
Practical Relief Strategies for Nighttime Itch
Environmental control is the first line of defense. Keep your bedroom cool (between 65–68°F / 18–20°C) and use a humidifier to maintain humidity around 50%. Lower temperatures reduce skin vasodilation and slow the release of itch mediators. Apply a thick emollient (petroleum jelly, ceramide cream, or shea butter) immediately after bathing — within three minutes of patting dry — to lock in moisture before transepidermal water loss begins. Switch to fragrance-free detergent and avoid synthetic sleepwear; 100% cotton or bamboo fabric reduces friction-induced itch. Non-sedating antihistamines (cetirizine, fexofenadine) taken in the morning help blunt histamine-driven itch throughout the day. Sedating antihistamines like diphenhydramine may help temporarily but cause next-day grogginess and lose effectiveness with nightly use — not ideal for chronic conditions. Topical calcineurin inhibitors (tacrolimus, pimecrolimus) are particularly effective for eczema night itch as they suppress T-cell activity directly. For scabies, permethrin 5% cream applied overnight and washed off in the morning treats the infestation itself. Cool, damp compresses provide immediate local relief for 15–20 minutes. Cognitive behavioral strategies — distraction, mindfulness — reduce the amplification of itch signals when lying awake in a quiet room.
Key Symptoms
- Itch that intensifies after 9 PM regardless of skin appearance
- Disrupted sleep from scratching cycles
- Visible scratch marks, excoriations, or broken skin in the morning
- Eczema, psoriasis, or hives flaring visibly before bedtime
- Generalized itch with no rash (may signal systemic disease)
- Scabies: intense itch between fingers, wrists, and body folds
Treatment Options
- Apply thick emollient within 3 minutes of bathing before bed
- Keep bedroom cool (65–68°F) and use a humidifier at 50% humidity
- Non-sedating antihistamines (cetirizine or fexofenadine) taken in the morning
- Cool compresses on affected areas for 15–20 minutes at night
- Wear 100% cotton or bamboo sleepwear; avoid synthetic fabrics
- See a doctor if systemic disease (liver, kidney, lymphoma) is suspected
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.