When Is a Rash Dangerous?
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
March 7, 2026
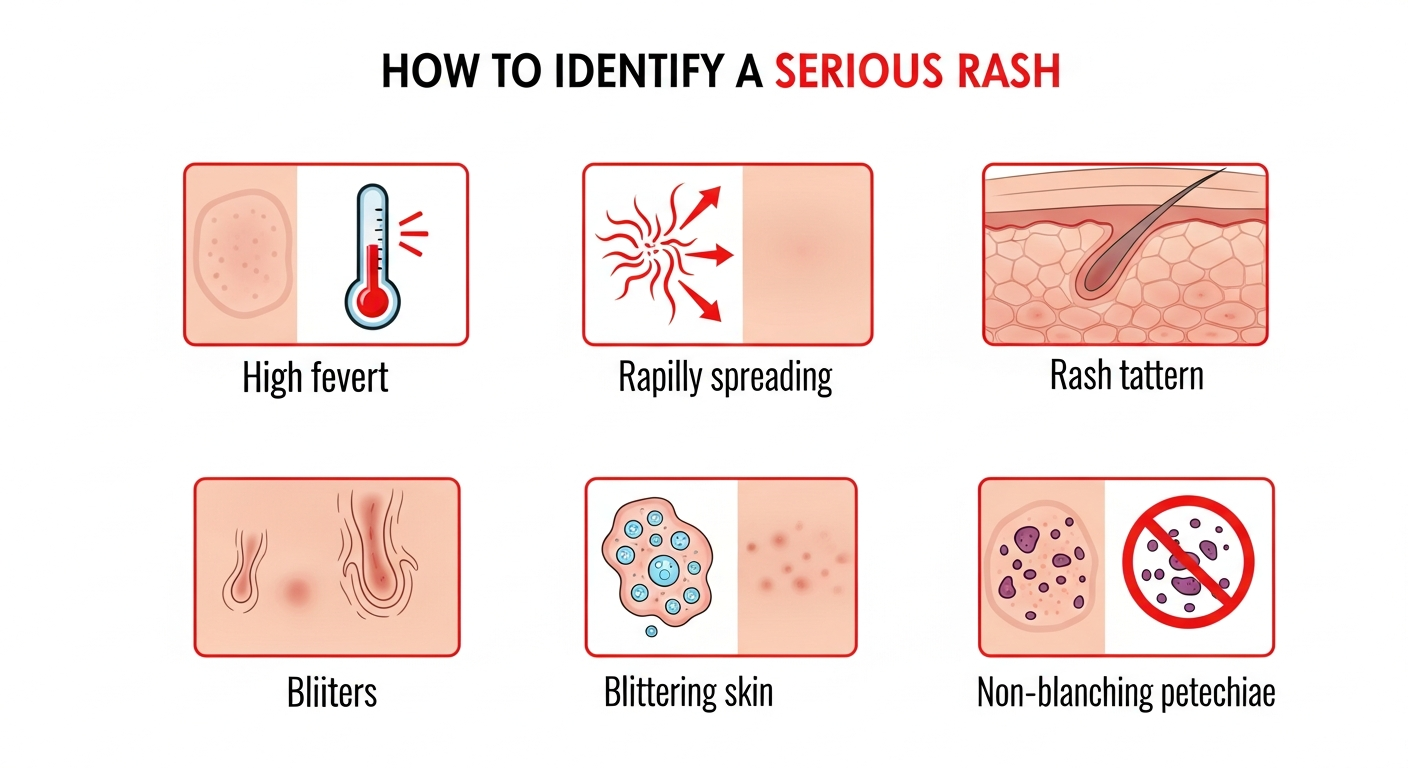
A rash becomes dangerous when it signals a life-threatening underlying process — infection, severe allergic reaction, drug reaction, or vascular emergency. The five features that make any rash immediately dangerous are: (1) it doesn't blanch when pressed, indicating blood has leaked from damaged vessels; (2) it is accompanied by fever above 103°F (39.4°C); (3) facial, tongue, or throat swelling is present; (4) it is rapidly spreading across large body areas within hours; and (5) it involves large-area blistering, especially near the eyes or mouth. Meningococcal disease, anaphylaxis, Stevens-Johnson Syndrome, toxic shock syndrome, and necrotizing fasciitis are the key diagnoses behind truly dangerous rashes. In contrast, the vast majority of rashes — contact dermatitis, hives, heat rash, eczema flares — are uncomfortable but not dangerous. Knowing which category your rash falls into determines whether you need emergency care now, a doctor visit this week, or simply time and basic treatment.
Quick Medical Summary
Life-Threatening Conditions That Cause Dangerous Rashes
Meningococcal septicemia is one of the most feared rash-associated emergencies. The characteristic non-blanching purpuric rash begins as small pink macules that rapidly transform into dark purple spots (purpura) and large coalescing bruises. Accompanying symptoms include high fever, severe headache, neck stiffness, photophobia, and confusion. Without IV antibiotics within hours, mortality is high. Apply the glass test (press a glass against the rash) — a meningococcal rash remains visible through the glass; benign rashes disappear. Anaphylaxis causes sudden, widespread urticaria, facial swelling, throat tightening, and difficulty breathing, typically within 5–30 minutes of allergen exposure. The skin component — generalized hives — is dangerous not in isolation but because it signals systemic anaphylaxis that can close the airway. Epinephrine (adrenaline) auto-injector (EpiPen) is the life-saving treatment. Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) are severe drug reactions causing the skin to blister and peel, as if burned, covering from 10% (SJS) to more than 30% (TEN) of body surface area. Mucous membranes of the eyes, mouth, and genitals are affected. Mortality of TEN exceeds 30%. Stop the causative drug immediately and seek emergency care. Toxic shock syndrome (TSS), caused by bacterial toxin release from Staph aureus or Group A Strep, causes a sunburn-like diffuse rash with fever, low blood pressure, and multi-organ involvement.
The Danger Signs to Know for Every Rash
Commit these seven warning signs to memory — any one of them warrants emergency evaluation, not a 'wait and see' approach. First: non-blanching rash — press glass or finger against the rash; if it stays visible/colored, seek emergency care immediately. Second: fever above 103°F (39.4°C) combined with any rash, particularly in children. Third: throat, tongue, or facial swelling — even mild swelling warrants immediate emergency attention as the airway can close rapidly. Fourth: rash spreading visibly within hours, especially with fever. Fifth: rash involving the eyes, mouth, or genitals, particularly if blisters are present. Sixth: the skin is painful to touch (most dangerous rashes are painful, not just itchy — necrotizing fasciitis and SJS are painful). Seventh: the patient has altered consciousness, confusion, extreme drowsiness, or cannot be woken normally alongside a rash. A secondary set of concerning signs that warrant urgent same-day evaluation (not necessarily emergency): rash in a newborn under 3 months; rash in an immunocompromised patient (cancer, HIV, organ transplant, chemotherapy); rash that started immediately after taking a new medication, especially antibiotics or NSAIDs; rash that has turned from pink to purple.
Rashes That Look Scary But Usually Aren't Dangerous
Many rashes are alarming in appearance but fundamentally benign. Petechiae (pinpoint red spots) from physical causes — coughing violently, weightlifting, or vomiting — are caused by pressure rupturing tiny capillaries and are not the same as meningococcal petechiae; they occur in a localized distribution (face and neck from vomiting, for example) without fever and resolve harmlessly. Erythema multiforme presents with distinctive target-shaped lesions (concentric rings of color change) and looks alarming but mild forms are usually triggered by herpes simplex virus and resolve spontaneously within 2–4 weeks. However, severe erythema multiforme major can progress to SJS — any mucosal involvement warrants evaluation. Pityriasis rosea begins with a single 'herald patch' followed by a widespread papulosquamous eruption across the trunk — it looks dramatic but is self-limiting, resolving within 6–12 weeks without treatment. Lichen planus produces shiny, flat-topped purple papules that look unusual and can involve the mouth, but is not dangerous in its cutaneous form. Port wine stains, haemangiomas, and other vascular birthmarks may look alarming but are not dangerous per se, though some (Sturge-Weber syndrome, PHACE syndrome) have associated systemic implications that require evaluation in infants.
Key Symptoms
- Non-blanching purple spots under glass pressure — immediate emergency
- Fever >103°F (39.4°C) with rash — urgent same-day evaluation
- Any throat, tongue, or facial swelling — immediate emergency
- Rash blistering over large areas or involving eyes/mouth
- Skin that is painful to touch rather than just itchy
- Confusion, altered consciousness, or neck stiffness alongside rash
Treatment Options
- Non-blanching rash or throat swelling: call 999/911 immediately
- Anaphylaxis: epinephrine auto-injector, then emergency services
- Suspected meningitis: antibiotics within the hour are life-saving
- SJS/TEN: stop all suspect medications; immediate hospital admission
- Toxic shock: IV antibiotics and intensive care support
- Benign rash: antihistamines, hydrocortisone cream, observe at home
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.