What Does a Fungal Rash Look Like?
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
January 15, 2026
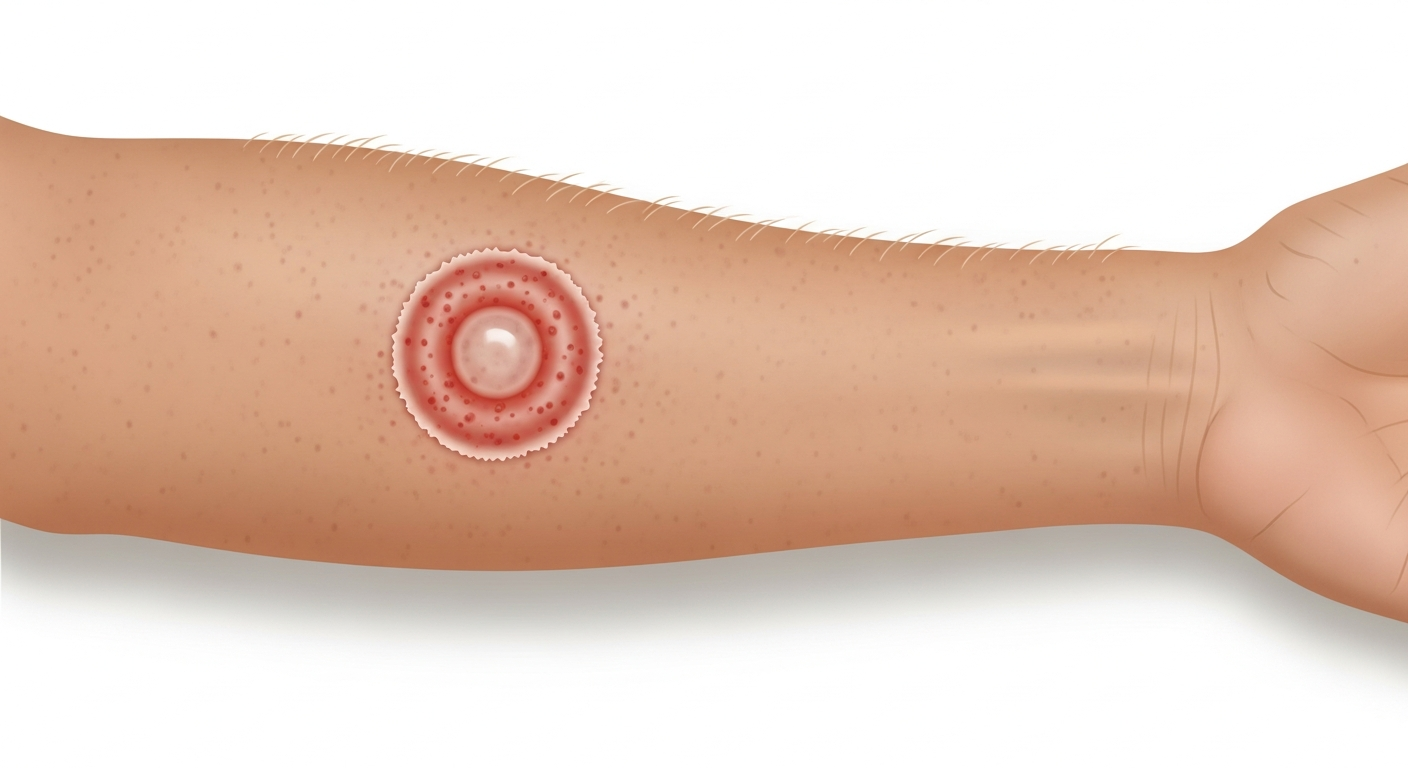
Fungal skin rashes have several characteristic features that distinguish them from bacterial, viral, and allergic rashes. The most classic sign is an annular (ring) shape with a raised, scaly, active outer border and a clearing or less-inflamed center — seen in ringworm (tinea corporis). The scaling of fungal rashes tends to be dry and powdery at the edges of lesions. Common fungal rashes include ringworm (body), athlete's foot (tinea pedis — scaly, macerated skin between toes), jock itch (tinea cruris — red, scaly rash in the groin crease), scalp ringworm (tinea capitis — scaly patches with hair loss), nail fungus (onychomycosis — thickened, yellow, crumbly nails), and candidal intertrigo (bright red, raw-looking rash in moist skin folds). The cardinal diagnostic error is applying topical steroid cream to a fungal rash — steroids suppress surface inflammation, creating a temporarily improved appearance while the fungus spreads unchecked, a condition called tinea incognito. When in doubt, a KOH skin scraping confirms or excludes fungal infection within minutes in a clinic setting.
Quick Medical Summary
Ringworm and Body Tinea: The Classic Fungal Ring
Tinea corporis (ringworm of the body) produces the archetypal fungal rash: one or more annular (ring-shaped) lesions with a raised, scaly outer border and a relatively clear, often hyperpigmented or less-inflamed center. The outer edge actively advances as the dermatophyte fungus grows centrifugally from the initial infection site. Multiple rings may coalesce into polycyclic (multi-ring) patterns. The surface within the ring is often slightly scaly or has residual hyperpigmentation from the resolving infection. Size ranges from 1–10 cm typically. Colors range from pink-red (active edge) to tan-brown (center) on light skin; darker skin tones may show more hyperpigmentation with less obvious redness. Ringworm is mildly to moderately itchy — significantly less itchy than eczema typically. The diagnosis is confirmed by KOH preparation of skin scrapings — a simple, quick, inexpensive office test that shows fungal hyphae (branching threads) under microscopy. Treatment: topical clotrimazole, miconazole, or terbinafine cream applied twice daily for 4 weeks (continuing for 2 weeks after apparent clearance). Tinea pedis (athlete's foot) appears on the feet — typically interdigital (between toes) maceration with white, waterlogged skin, scaling, and fissuring; or a diffuse, dry, scaly 'moccasin' distribution covering the sole and heel; or a vesicular form with intensely itchy blisters on the instep.
Candidal Rashes: Yeast in Moist Skin Folds
Candidal skin infections look distinctly different from dermatophyte (tinea) infections. Candida albicans thrives in warm, moist environments — skin folds, the diaper area, under the breasts, and in the groin. Candidal intertrigo produces a bright red, beefy-red or deep pink raw-looking rash in the depths of skin folds, often with satellite lesions — smaller red papules and pustules scattered just beyond the main rash border. The satellite lesion pattern is highly characteristic of candidal infection and helps distinguish it from intertrigo (friction rash), inverse psoriasis, or erythrasma. The affected skin may be moist and macerated (soft, white, and wrinkled at the fold's depth) or dry and scaling at the edges. Oral thrush (candidal stomatitis) produces white, cottage cheese-like plaques on the tongue, inner cheeks, and palate that can be scraped off revealing a raw red base — it is not a skin rash per se but indicates systemic immune suppression if occurring outside of newborns or antibiotic use. Candidal diaper rash in infants produces a bright red, sharply defined rash involving the skin folds of the groin crease (unlike irritant diaper rash, which typically spares the folds). Treatment: topical clotrimazole or miconazole cream to skin candidiasis; keep area dry and ventilated; treat predisposing factors (antibiotic use, diabetes, immunosuppression).
How to Distinguish Fungal Rash from Eczema and Psoriasis
The most common diagnostic error in dermatology is treating ringworm as eczema with topical corticosteroid — creating tinea incognito (steroid-modified ringworm), where the ring is partially suppressed but the fungal infection spreads over a wider, less defined area. Clues that a 'eczema' rash may actually be tinea: it affects only one side of the body (classic for tinea manuum — 'two feet one hand' syndrome); it has a subtly raised, advancing edge even within the larger scaly patch; it has not responded to two courses of topical steroids; it involves the scalp with scale and patchy hair loss (tinea capitis, not seborrheic dermatitis). Eczema vs. ringworm: eczema is bilaterally symmetric (both elbows, both knees, both sides of the neck), chronically recurrent with clear history, intensely itchy (more than ringworm), doesn't have a ring shape with cleared center, and responds to corticosteroids. Psoriasis vs. tinea: psoriasis plaques are thick, have silvery scale (rather than fine, powdery fungal scale), sharply defined borders, occur on the scalp/elbows/knees, and are not ring-shaped. Psoriasis affecting the scalp (without hair loss) can be confused with tinea capitis (with hair loss). KOH scraping definitively resolves diagnostic uncertainty and should be performed before prescribing topical steroids for any scaling, rash.
Key Symptoms
- Ring shape with raised scaly border and clearing center (ringworm/tinea corporis)
- Scaling, maceration, and fissuring between toes (athlete's foot/tinea pedis)
- Bright red rash with satellite papules in skin folds (candidal intertrigo)
- Scaly patches with patchy hair loss on scalp (tinea capitis)
- Thickened, yellow, crumbly, separated nails (onychomycosis)
- Red, scaly rash in groin crease with clear central border (tinea cruris/jock itch)
Treatment Options
- Tinea (ringworm, athlete's foot, jock itch): topical clotrimazole or terbinafine 2× daily for 4 weeks
- Tinea capitis: oral griseofulvin or terbinafine — topical insufficient for scalp
- Onychomycosis: oral terbinafine for 6 weeks (fingernails) or 12 weeks (toenails)
- Candidal intertrigo: clotrimazole cream + keep dry + antifungal powder
- KOH skin scraping to confirm diagnosis before any steroid treatment
- Never apply steroid cream to unconfirmed ring rash — risk of tinea incognito
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.