What Does Eczema Look Like?
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
December 15, 2025
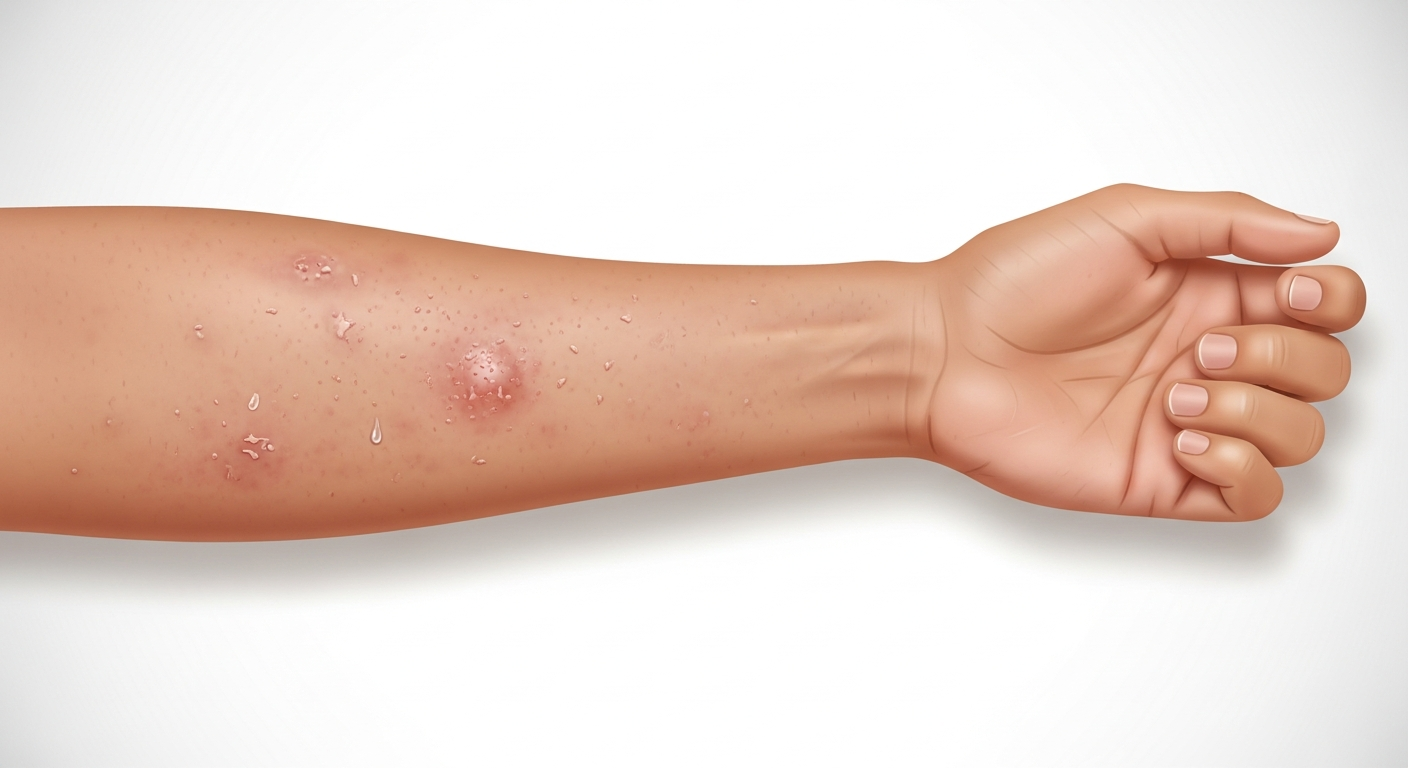
Eczema (atopic dermatitis) appears as patches of intensely itchy, inflamed skin that varies significantly in appearance depending on the stage of the flare, the patient's age, and skin tone. In an active flare, eczema typically looks red, swollen, and either dry and scaly or wet and weeping — sometimes both in different areas simultaneously. On fair skin, the redness is obvious; on darker skin tones, eczema often appears as darker purple-brown or hyperpigmented patches with the same texture and itch characteristics. The skin surface may be dry and rough with fine scales, or may develop vesicles (tiny fluid-filled blisters) that rupture and ooze a clear or yellowish fluid. After an acute phase, eczema skin becomes dry, thickened, and darker — a process called lichenification — from repeated scratching. In infants, eczema classically appears on the cheeks and scalp. In children, it favors the inner elbow creases, behind the knees, and the wrists. In adults, it most commonly affects the hands, neck, face, and flexural areas.
Quick Medical Summary
Eczema Appearance by Age and Location
Infantile eczema (0–2 years) typically begins on the cheeks with symmetrical red, rough, scaling patches that are intensely itchy — the baby rubs their face against bedding. The scalp develops similar scaling. In severe cases, the rash spreads to the trunk, arms, and legs. The diaper area is usually spared (moisture in that area paradoxically protects). Childhood eczema (2–12 years) characteristically migrates to the flexural surfaces — the creases inside the elbows (antecubital fossae) and behind the knees (popliteal fossae) — along with the wrists, ankles, and around the neck. The skin in these areas becomes thickened, leathery, and darker from chronic scratching — lichenification. Adolescent and adult eczema often concentrates on the hands (causing deeply cracked, painful, weeping hand eczema), the eyelids (an area extremely sensitive to allergens in cosmetics and preservatives), the neck, and the face. Hand eczema is particularly debilitating for people who work with wet hands (healthcare workers, food workers). Nummular eczema presents as coin-shaped (discoid) patches, commonly on the arms and legs, without the flexural predilection of atopic dermatitis. Dyshidrotic eczema produces tiny, intensely itchy vesicles (blisters) along the sides of the fingers, palms, and soles — often flaring in spring and autumn.
How Eczema Looks on Different Skin Tones
Medical education has historically overrepresented eczema in fair-skinned individuals, but eczema affects all ethnicities and has specific presentations in darker skin tones that practitioners must recognize. On light skin (Fitzpatrick types I–III), active eczema is bright red, clearly demarcated from surrounding normal skin, and may have a pink halo. Post-inflammatory hyperpigmentation is mild. On medium skin tones (Fitzpatrick IV), eczema active lesions appear pinkish-red to dark red; post-inflammatory hyperpigmentation after flares resolves is more prominent and takes months to fade. On darker skin tones (Fitzpatrick V–VI), the redness of active eczema may be subtle or difficult to detect clinically — lesions appear more as darker purple-brown or ashy gray patches with similar texture changes (dryness, scaling, thickening) to lighter skin presentations. The itch and skin thickening are identical across skin tones; the color difference is primarily in the inflammatory phase. Post-inflammatory hyperpigmentation is the most visible and persistent feature in darker skin, often lasting months to years after the active eczema is controlled. Vitiligo (loss of pigment) can be confused with post-inflammatory hypopigmentation from healed eczema in darker skin — both leave lighter patches, but vitiligo patches are completely depigmented while eczema hypopigmentation retains some pigment.
How to Distinguish Eczema from Similar Rashes
Eczema is most commonly confused with psoriasis, ringworm, contact dermatitis, and seborrheic dermatitis. Psoriasis produces well-defined, thick, silver-scaled plaques on the scalp, elbows, knees, and lower back — the scale is thicker and more silvery than eczema's finer, whiter scale. Psoriasis plaques have sharply defined borders while eczema patches are poorly bordered and merge with normal skin. Psoriasis is less intensely itchy than eczema and does not weep or ooze. Ringworm (tinea corporis) is most commonly misdiagnosed as eczema. The key distinguishing features: ringworm has a distinct ring shape with a raised, scaly, active outer border and a clearing or darker center; eczema does not form rings. Applying topical steroids to ringworm suppresses surface inflammation, making it look temporarily better but allowing the fungal infection to spread — called 'tinea incognito.' A KOH (potassium hydroxide) skin scraping test distinguishes fungal from inflammatory causes. Contact dermatitis follows the precise shape of allergen contact (e.g., a rectangular watch-shaped patch under a nickel watch buckle) — eczema doesn't conform to object shapes. Seborrheic dermatitis affects oil-rich areas (scalp, nose folds, eyebrows, chest) with yellowish-white scale, while eczema has whiter scale and occurs in flexural areas.
Key Symptoms
- Intensely itchy red-to-purple patches in skin creases (elbows, knees, neck)
- Dry, rough, scaly skin or weeping, crusted lesions during active flares
- Skin thickening and darkening (lichenification) from chronic scratching
- Tiny blisters (vesicles) on fingers or palms in dyshidrotic type
- Face and scalp involvement in infants with symmetrical red patches
- Hand eczema: deeply cracked, painful, weeping skin on palms and fingers
Treatment Options
- Daily thick emollient (petroleum jelly, ceramide cream) within 3 minutes of bathing
- Topical corticosteroids (hydrocortisone 1% OTC; prescription strength for flares)
- Topical calcineurin inhibitors (tacrolimus, pimecrolimus) for sensitive areas
- Oral antihistamines for nighttime itch management
- Biologic therapy (dupilumab/Dupixent) for moderate-to-severe cases
- Identify and avoid personal triggers (fragrances, dust mites, certain foods)
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.