What Causes a Rash on the Hands?
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
January 26, 2026
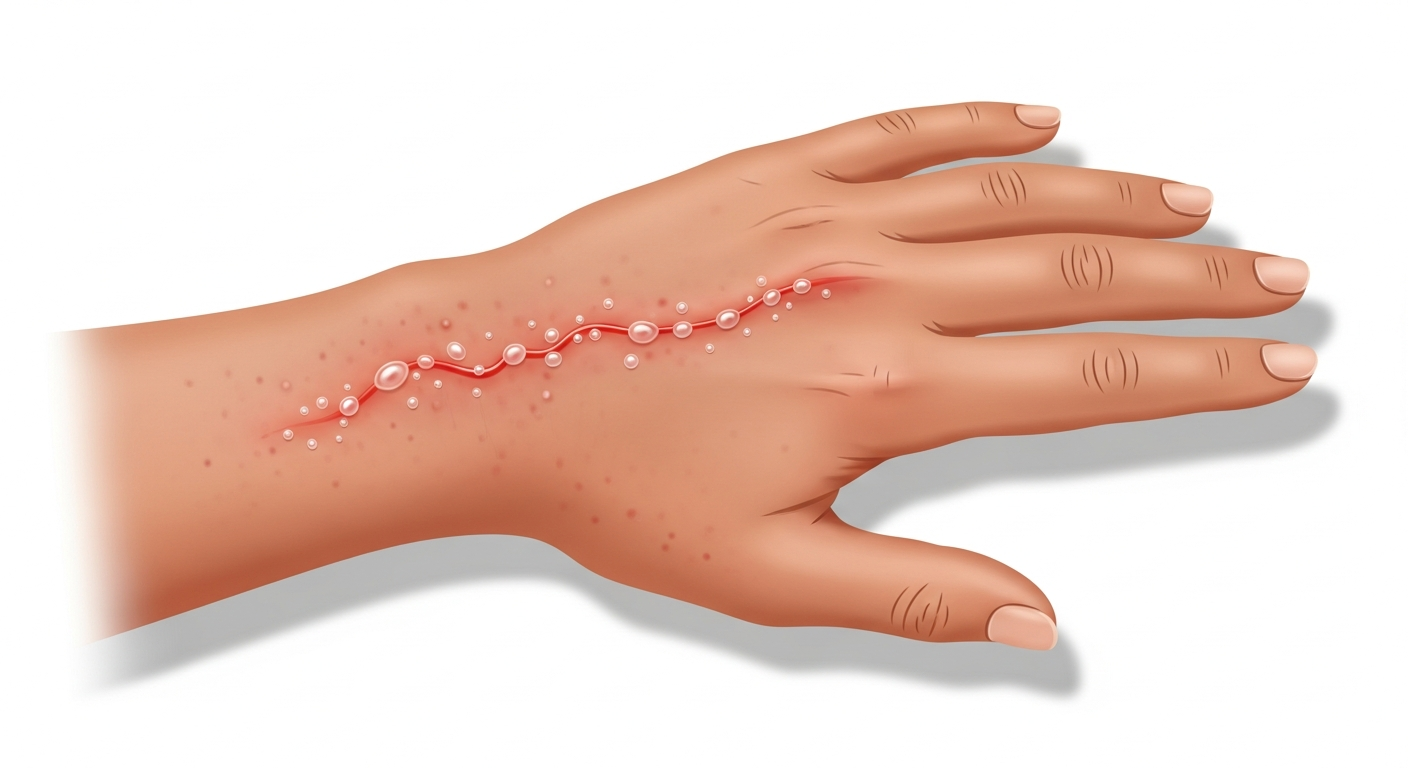
Hand rashes are among the most common dermatological complaints, and the hands are exposed to an extraordinary range of potential irritants and allergens every day — soaps, cleaning products, metals, rubber gloves, foods, and environmental allergens. The most frequent causes of hand rash are contact dermatitis (irritant or allergic), dyshidrotic eczema (tiny blisters along the fingers and palms), hand eczema (atopic), psoriasis on the palms, tinea manuum (fungal hand infection), and scabies (which classically involves the webs between fingers). Occupational hand rashes are a major problem for healthcare workers, hairdressers, mechanics, food handlers, and builders who have prolonged wet work or chemical exposure. Key diagnostic clues include the precise location on the hand (dorsum vs. palms vs. fingertips vs. web spaces), whether blisters are present, and whether both hands are equally affected or just one.
Quick Medical Summary
The Most Common Hand Rash Causes
Irritant contact dermatitis is the leading cause of hand rashes worldwide, particularly in people who wash their hands frequently or work with water, chemicals, or cleaning products. Repeated exposure to soap, detergent, disinfectant, and water strips the skin's lipid barrier, causing redness, dryness, cracking, and scaling — predominantly on the fingertips and the dorsum (back) of the hands. Healthcare workers and food handlers are disproportionately affected. Allergic contact dermatitis requires prior sensitization: the rash appears 24–72 hours after allergen contact, itches intensely, may blister, and corresponds exactly to the area of contact. Common hand allergens include nickel (jewellery), rubber accelerators (latex gloves), fragrance, preservatives (methylisothiazolinone in soaps and wipes), and acrylates (in nail products and adhesives). Dyshidrotic eczema (pompholyx) produces tiny, deep-seated vesicles (blisters) along the lateral sides of the fingers and on the palms, with intense itch and burning. It is exacerbated by sweating, stress, and nickel exposure. The blisters eventually dry and peel, leaving cracked, sore skin. It affects both hands typically but can be asymmetric.
Less Common but Important Causes
Psoriasis on the palms (palmoplantar psoriasis) produces thick, yellow-scaled plaques on the palms and soles — often with fissuring (deep, painful cracks). It is notoriously resistant to topical treatment and significantly impairs hand function. Unlike most psoriasis, palmoplantar psoriasis may lack plaques elsewhere on the body, making diagnosis more challenging. Tinea manuum (ringworm of the hand) is frequently misdiagnosed as eczema or psoriasis. It typically affects one hand only (the 'two feet, one hand' pattern with tinea pedis on both feet), presents as dry, scaling skin with a slightly raised active border, and confirms on KOH preparation. Applying topical steroids to tinea manuum (mistaking it for eczema) accelerates fungal spread dramatically — always suspect tinea manuum in hand rash affecting only one hand. Scabies classically involves the web spaces between fingers with thin, thread-like burrow lines (0.5–1 cm grey lines). Intense itching worse at night is characteristic. Hand warts (verruca vulgaris) may be mistaken for a rash when multiple warts appear — look for firm, rough papules with disrupted skin lines and black dots (thrombosed capillaries). Porphyria cutanea tarda causes fragile, blistering skin on sun-exposed hand skin — associated with liver disease, alcohol use, and certain medications.
Treatment by Cause
Treating hand rash correctly requires accurate diagnosis — the treatments for different causes are not interchangeable and some are actively contraindicated for certain diagnoses. For irritant contact dermatitis: reduce wet work, use thick emollient barrier cream before tasks, switch to fragrance-free gentle cleansers, and wear vinyl gloves (not latex or rubber, which can cause allergic contact dermatitis) for wet work. Topical corticosteroids (betamethasone valerate, clobetasol) clear active inflammation. For dyshidrotic eczema: mid-to-high potency topical steroids during active vesicle phase; emollients during resolution; avoid nickel; manage stress. Severe cases may need systemic immunosuppression (ciclosporin, dupilumab). For tinea manuum: topical terbinafine or clotrimazole twice daily for 4–6 weeks; always treat concomitant tinea pedis or the hand will be rapidly reinfected from the feet. For palmoplantar psoriasis: high-potency topical steroids under occlusion; PUVA phototherapy; acitretin; biologics for severe disease. For allergic contact dermatitis: the allergen must be identified (patch testing) and permanently avoided — even trace exposures can perpetuate the rash. Barrier hand cream with zinc oxide before exposure helps, but allergen avoidance is the definitive solution.
Key Symptoms
- Cracking, dryness, and redness on fingertips and hand dorsum (irritant dermatitis)
- Intensely itchy tiny blisters along finger sides and palms (dyshidrotic eczema)
- Thick, yellow, cracked plaques on palms (palmoplantar psoriasis)
- Scaly rash on one hand only, often with both feet affected (tinea manuum)
- Web-space burrow lines with severe nighttime itch (scabies)
- Rash matching exact shape of jewelry, glove, or product contact (allergic dermatitis)
Treatment Options
- Irritant dermatitis: barrier cream, vinyl gloves for wet work, emollient, gentle cleansers
- Dyshidrotic eczema: topical steroids during active phase, emollients, nickel avoidance
- Tinea manuum: topical or oral antifungals for 4–6 weeks; treat feet simultaneously
- Allergic contact dermatitis: patch test to identify allergen; permanent avoidance
- Palmoplantar psoriasis: high-potency steroids under occlusion; referral to dermatologist
- Scabies: permethrin 5% cream to all body surfaces; treat all household contacts
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.