What Causes a Rash on the Face?
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
October 30, 2025
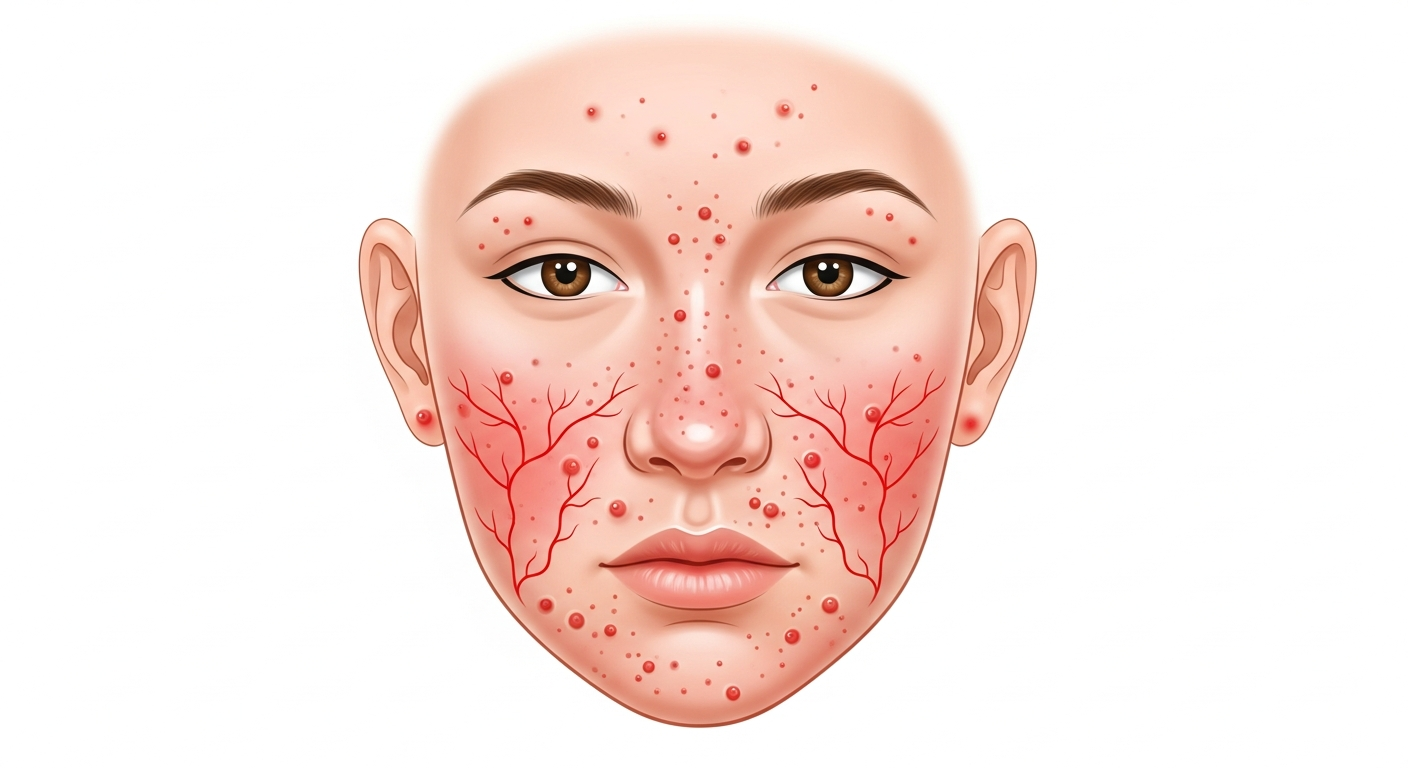
Facial rashes are common and often distressing because they are visible and socially impactful. The face has unique skin properties — high sebaceous (oil) gland density, thinner skin than the body, and greater sun exposure — that make it susceptible to specific conditions. The most frequent causes of facial rash include rosacea (flushing, redness, and papules on the central face), seborrheic dermatitis (flaking, yellowish rash in the creases of the nose, eyebrows, and along the hairline), perioral dermatitis (small papules and pustules around the mouth, often triggered by inhaled or topical steroids), contact dermatitis from cosmetics or sunscreen, atopic eczema (especially around the eyes and cheeks), and the butterfly rash of lupus (symmetrical redness across the cheeks and nose bridge). Accurate diagnosis is critical because treatments differ significantly — topical steroids, for example, may worsen rosacea and perioral dermatitis while being effective for eczema.
Quick Medical Summary
Rosacea, Seborrheic Dermatitis, and Perioral Dermatitis
These three conditions account for the majority of adult facial rashes and are frequently confused with each other and with eczema. Rosacea affects the central face — cheeks, nose, chin, and forehead — and presents in four subtypes: erythematotelangiectatic rosacea (persistent facial redness and flushing with visible blood vessels), papulopustular rosacea (red papules and pustules resembling acne but without comedones), phymatous rosacea (skin thickening, particularly of the nose — rhinophyma), and ocular rosacea (eye involvement with redness and irritation). Triggers include heat, alcohol, spicy food, and sun exposure. Key distinguishing feature: rosacea never has comedones (blackheads/whiteheads). Seborrheic dermatitis affects oily areas of the face — the creases beside the nose (nasolabial folds), eyebrows, ears, and forehead — producing yellowish-white, flaking scale on a red base. It is caused by an inflammatory response to Malassezia yeast overgrowth and improves with antifungal treatment (ketoconazole cream, zinc pyrithione). Perioral dermatitis produces clustered small papules and pustules specifically around the mouth (perioral), often sparing a narrow zone immediately adjacent to the lip border. It is strongly associated with prolonged use of topical or inhaled corticosteroids. Stopping the steroid (which may initially worsen the rash) and treating with topical metronidazole or oral doxycycline are standard.
Eczema, Contact Dermatitis, and Lupus on the Face
Facial eczema most commonly affects the eyelids (eyelid eczema) and the skin around the eyes, producing intensely itchy, scaly, thickened skin that worsens with cosmetics, eye drops, and contact lens solutions — allergens that patch testing commonly identifies. In children, eczema affects the cheeks (infantile eczema) and fades from the face as children age. Adult facial eczema is usually identified by its location around the eyes, associated atopic history (asthma, hay fever), and response to mild topical steroids. Facial contact dermatitis from cosmetics is underdiagnosed. Common culprits include fragrances (in moisturisers, foundations, sunscreens), preservatives (methylisothiazolinone, parabens), hair dye (para-phenylenediamine/PPD spreading from hairline to forehead and ears), and nickel in eyeglass frames (affecting the nose bridge and temples). Patch testing identifies the specific allergen, enabling permanent avoidance. The malar rash of systemic lupus erythematosus (SLE) appears as a fixed, flat or slightly raised red rash across the cheeks and nose bridge in a 'butterfly' (malar) distribution — typically sparing the nasolabial folds, which distinguishes it from rosacea and seborrheic dermatitis which affect those folds. The lupus rash is photosensitive (worsens with sun exposure) and is associated with systemic symptoms: joint pain, fatigue, oral ulcers, and abnormal blood tests.
Sun-Related, Infectious, and Hormonal Facial Rashes
Sun exposure affects facial skin in multiple ways. Polymorphic light eruption (PLE) causes itchy papules, vesicles, or plaques on sun-exposed facial and chest skin within hours of UV exposure, typically in spring and early summer as the skin readjusts to sun. It resolves without sun avoidance and gradually desensitizes over the summer. Photocontact dermatitis from sunscreen chemicals produces a rash specifically on sun-exposed facial skin rather than shaded areas (under chin, behind ears), distinguishing it from other facial rashes. Sunburn causes erythema, pain, and eventually peeling — significant sun damage cumulates over decades, increasing the risk of actinic keratoses (pre-cancerous rough spots) and skin cancer. Facial impetigo in children produces honey-colored crusted sores around the nose and mouth — a bacterial infection requiring antibiotic treatment. Herpes simplex (cold sore/fever blister) causes clusters of small blisters on the lip border that recur in the same location, driven by the sun, stress, or illness. Herpes zoster (shingles) on the face follows a dermatomal pattern — unilateral (one-sided), following the ophthalmic or maxillary branch of the trigeminal nerve, with burning pain preceding the blisters by 1–3 days. Melasma — symmetrical brown-gray patches on cheeks, forehead, and upper lip — is a hormonal hyperpigmentation (not a rash) associated with pregnancy, oral contraceptives, and sun exposure; it requires sun protection and topical depigmenting agents.
Key Symptoms
- Central face redness, flushing, and papules without comedones (rosacea)
- Yellowish scale in nose creases, eyebrows, and ears (seborrheic dermatitis)
- Papules and pustules around the mouth, sparing lip border (perioral dermatitis)
- Itchy, scaly rash around the eyes (facial eczema/eyelid eczema)
- Butterfly-shaped redness across cheeks and nose bridge (lupus malar rash)
- Honey-crusted sores around the nose and mouth in children (impetigo)
Treatment Options
- Rosacea: azelaic acid, topical metronidazole; avoid triggers; laser for telangiectasia
- Seborrheic dermatitis: ketoconazole 2% cream; zinc pyrithione wash
- Perioral dermatitis: stop topical steroids; topical metronidazole; oral doxycycline
- Facial eczema: mild topical steroid; calcineurin inhibitors (tacrolimus) for eyelid
- Facial contact dermatitis: patch test; allergen avoidance; topical steroid
- Lupus malar rash: antimalarials (hydroxychloroquine); sun protection; rheumatology referral
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.