Rash That Looks Like a Ring: What Is It?
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
March 19, 2026
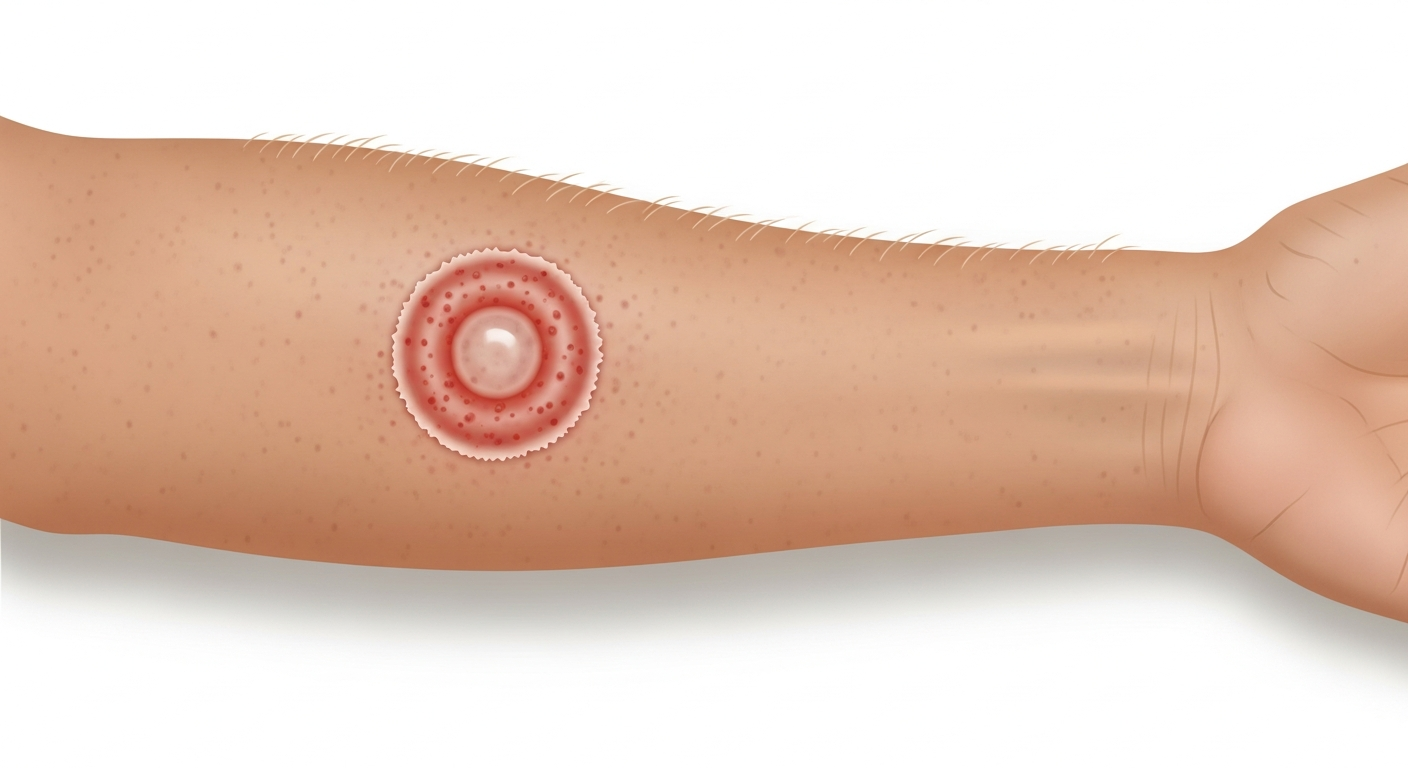
A ring-shaped rash has a distinctive annular (circular) pattern with a raised or active outer border and a clearing or different-colored central area. The most important diagnoses to consider are ringworm (tinea corporis), Lyme disease (erythema migrans), granuloma annulare, nummular eczema (which can appear ring-like as it clears centrally), and erythema multiforme. The cause matters enormously — ringworm is a fungal infection treated with antifungals, Lyme disease is a bacterial infection requiring antibiotics, granuloma annulare is an inflammatory condition treated with steroids, and erythema multiforme is usually viral and self-limiting. Never apply a topical steroid to a ring rash without knowing the diagnosis — steroids dramatically worsen ringworm by suppressing the superficial inflammation while allowing the fungus to spread unchecked, a phenomenon called tinea incognito.
Quick Medical Summary
Ringworm (Tinea Corporis): The Classic Ring Rash
Despite its alarming name, ringworm has nothing to do with worms — it is a superficial fungal infection caused by dermatophytes (Trichophyton, Microsporum, or Epidermophyton species). The characteristic ring shape develops because the fungus grows centrifugally from the initial infection point, with the active outer edge representing the growing fungal front and the clearing center representing areas where the immune response has partially cleared the infection. Key features: well-defined ring with a raised, scaly, often slightly blistering outer border; central clearing or hyperpigmentation; may have multiple coalescing rings creating complex patterns; mildly to moderately itchy; affects any body area but most commonly the trunk, arms, and groin. Diagnosis is confirmed by KOH (potassium hydroxide) microscopy of skin scrapings — fungal hyphae appear as branching threads under the microscope. Treatment: topical clotrimazole, terbinafine, or miconazole cream twice daily for 4 weeks. Complete the full course — stopping when it 'looks better' guarantees recurrence. Tinea capitis (ringworm of the scalp) requires oral antifungal (griseofulvin, terbinafine) as topical antifungals cannot penetrate the hair follicle.
Lyme Disease Rash (Erythema Migrans)
Erythema migrans (EM) is the hallmark rash of Lyme disease, appearing in 70–80% of infected individuals 3–30 days after a bite from an infected Ixodes tick. The classic description — a 'bull's-eye' rash with concentric rings of redness separated by clearing — occurs in only about 20% of cases. More commonly, EM appears as a uniformly red, expanding oval or round patch, often 5–70 cm in diameter. Key distinguishing features from ringworm: EM expands rapidly (growing 1–2 cm per day), has a smooth (not raised, scaly) border, is warm to touch, and is usually found near the tick bite site (often hairline, groin, axilla, or behind the knee — favored tick attachment sites). It is typically mildly warm and may be slightly tender. There is no itch or scale in the early phase. EM may be accompanied by flu-like symptoms (fatigue, fever, muscle aches). Any ring-shaped rash that appeared after outdoor activity in tick-endemic areas (Northeast USA, upper Midwest, Europe) should be evaluated urgently — Lyme disease responds excellently to early antibiotic treatment (doxycycline) but can cause serious complications if delayed.
Other Ring-Shaped Rashes
Granuloma annulare produces smooth, skin-colored or slightly pinkish ring-shaped plaques, most commonly on the dorsum (back) of the hands, feet, elbows, and knees. Crucially, it is NOT scaly — the ring border is smooth and raised rather than scaly and flaking. It is caused by an immune reaction of unclear etiology, is benign, and often resolves spontaneously over 1–2 years. Intralesional corticosteroid injection accelerates resolution. Nummular eczema (discoid eczema) produces coin-shaped, intensely itchy patches that may develop central clearing as they begin to resolve, appearing transiently ring-like. Active nummular eczema patches have an oozing, crusted surface rather than a smooth or scaly ring border. Erythema multiforme causes target lesions — three zones of color (a dark or blistered center, a pale edematous ring, and an outer red ring) — most commonly on the palms, soles, and extremities. Mild forms are usually triggered by herpes simplex virus and resolve in 2–4 weeks. Pityriasis rosea begins with a single 'herald patch' that may look ring-like, followed by an eruption of similar but smaller lesions along skin tension lines across the trunk. Fixed drug eruption can produce annular (ring-shaped) patches in the same location every time the causative drug is taken.
Key Symptoms
- Ring with raised, scaly, active outer border and central clearing (ringworm)
- Smooth, rapidly expanding red oval patch at tick bite site (Lyme disease EM)
- Smooth, skin-colored raised ring on hands or feet, no scale (granuloma annulare)
- Coin-shaped itchy, crusted patch with central clearing (nummular eczema)
- Three-zone target lesion on palms and soles (erythema multiforme)
- Ring rash returning in same location after taking a specific medication (fixed drug)
Treatment Options
- Ringworm: topical clotrimazole or terbinafine for full 4 weeks
- Lyme disease EM: oral doxycycline 100mg twice daily for 10–21 days — urgent
- Granuloma annulare: intralesional steroids or watchful waiting
- Nummular eczema: topical corticosteroids, emollients, antihistamines for itch
- Erythema multiforme: treat underlying HSV trigger; antihistamines for comfort
- Never apply steroid cream to an undiagnosed ring rash — confirm diagnosis first
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.