How to Treat Heat Rash at Home
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
November 7, 2025
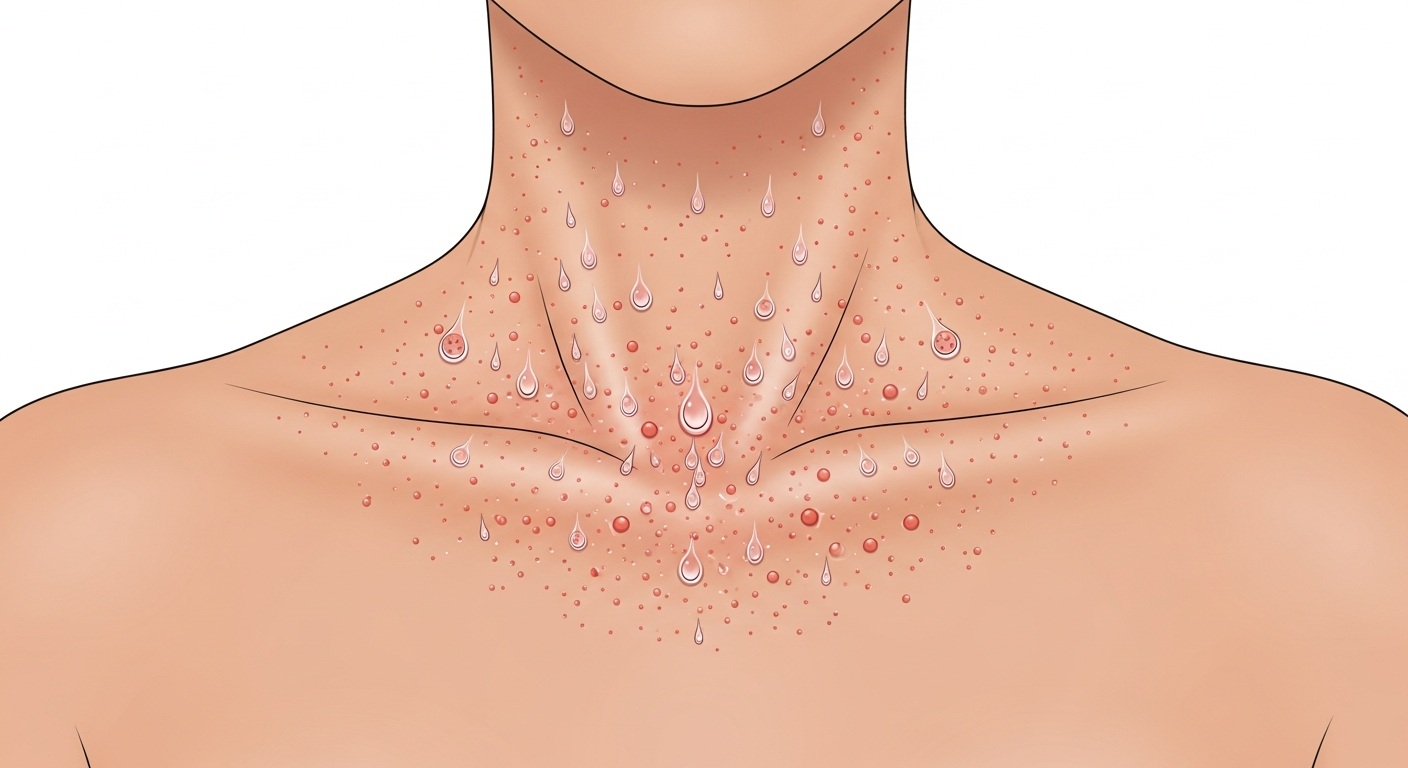
Heat rash (miliaria rubra) can be effectively treated at home in most cases by cooling the body, keeping the skin dry, and allowing blocked sweat glands to recover. The cause of heat rash is straightforward: excessive sweating in hot, humid conditions blocks sweat ducts, causing sweat to leak into surrounding skin layers and producing inflammation. The tiny red, prickly bumps (papules) most commonly appear in skin folds (neck, armpits, groin, under the breasts) and on the back, chest, and shoulders. The primary treatment is removing the heat source — move to an air-conditioned environment, remove tight or synthetic clothing, and take a cool shower. Most mild heat rash resolves within 3–4 days with proper cooling. Calamine lotion soothes the itching and drying effect, and hydrocortisone 1% cream reduces inflammation if the rash is particularly red and inflamed. Avoid thick, greasy emollients — they trap more heat and worsen blocked sweat glands.
Quick Medical Summary
Immediate Home Treatment Steps
The first and most effective step is cooling the body immediately. Move to an air-conditioned room or shaded area; the drop in ambient temperature reduces sweating and allows the blocked sweat glands to recover. Take a cool (not ice cold) shower — lukewarm water prevents the shock response that causes vessels to constrict, which can trap heat. After showering, pat (do not rub) the skin dry to avoid further trauma to already-irritated sweat glands. Change into loose-fitting, breathable clothing: 100% cotton or moisture-wicking athletic fabric allows air circulation and absorbs sweat without trapping it. Avoid nylon, polyester, and tight waistbands or bra straps, which compress skin and worsen occlusion of sweat ducts. Calamine lotion applied to the affected areas provides immediate relief — the zinc oxide in calamine is mildly astringent and absorbs excess moisture, while the cooling evaporation of the lotion soothes the prickly itch. Apply two to three times daily. Hydrocortisone 1% cream reduces the local inflammatory response that causes redness and itching; apply sparingly once or twice daily for up to 7 days. Do not use thick barrier creams, petroleum jelly, or heavy body lotions on heat rash — these trap further heat and moisture, obstructing sweat gland recovery.
Natural and Supplementary Home Remedies
Cool compresses provide instant localized relief: soak a clean cotton cloth in cool (not ice) water, wring it out, and apply to the rash for 15–20 minutes. Repeat as needed throughout the day. Do not apply ice directly to the rash — extreme cold can cause vasoconstriction and worsen skin irritation. Oatmeal baths have genuine evidence-based anti-inflammatory and anti-itch properties. Colloidal oatmeal (finely ground oat flour) is FDA-approved as a skin protectant. Add 1–2 cups of finely ground oatmeal to a lukewarm bath and soak for 15–20 minutes; pat dry gently afterward. Aloe vera gel — the clear gel from the inner leaf of the aloe plant — has mild anti-inflammatory and cooling properties. Apply pure aloe gel (without added alcohol or fragrance) to the rash two to three times daily. Evidence for aloe is modest but the anecdotal experience of relief is consistent and it has a good safety profile. Baking soda: a small amount dissolved in cool bath water can help reduce itch through its mild alkalizing effect on the skin surface. Use 3–4 tablespoons per bath. Note that undiluted baking soda applied directly to the skin is too alkaline and can irritate — always dilute. Ensure adequate hydration: drink enough water so urine is pale yellow. Dehydration concentrates sweat, increasing its irritant effect on blocked ducts.
Preventing Heat Rash from Returning
Once heat rash has cleared, targeted preventive measures can significantly reduce the likelihood of recurrence during hot weather or exercise. Clothing choice is the most impactful factor: wear loose, light, breathable fabrics that allow air circulation and wick moisture away from the skin. Avoid tight clothing in areas prone to heat rash (neck, armpits, groin, under breasts). Take cool showers after exercise or sweating before changing into dry clothing. Apply a light, non-occlusive dusting powder (cornstarch or medical-grade talc-free powder) to high-risk areas before activity to absorb moisture and reduce friction, two of the key precipitating factors. Time outdoor exercise for cooler parts of the day — early morning or evening — during heat waves. Use fans or air conditioning to keep sleep environments cool (below 72°F/22°C), as heat rash commonly develops at night in hot bedrooms. In infants — who are most vulnerable — monitor for overdressing: a baby should wear one more layer than an adult is comfortable in, not significantly more. Check the back of the neck to assess temperature — warmth without sweating is appropriate; sweating suggests overdressing. Infants with heat rash should be undressed, moved to a cool environment, and offered extra feeds for hydration.
Key Symptoms
- Tiny red, prickly bumps in skin folds (neck, armpits, groin, under breasts)
- Prickling or burning sensation rather than typical itch
- Rash appearing during hot, humid weather or after exercise
- Small blisters (miliaria crystallina) in very mild cases — clear and painless
- Deeper, pus-filled bumps (miliaria pustulosa) if secondarily infected
- Skin feels hot and sticky in the affected area
Treatment Options
- Move to a cool, air-conditioned environment immediately
- Cool shower and change to loose, breathable cotton clothing
- Calamine lotion 2–3 times daily for itch and moisture absorption
- Hydrocortisone 1% cream for up to 7 days to reduce inflammation
- Cool oatmeal bath for 15–20 minutes for widespread heat rash
- See a doctor if rash shows signs of infection: pus, increasing pain, fever
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.