Rash on Legs: Causes, Symptoms, and When to See a Doctor
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
December 4, 2025
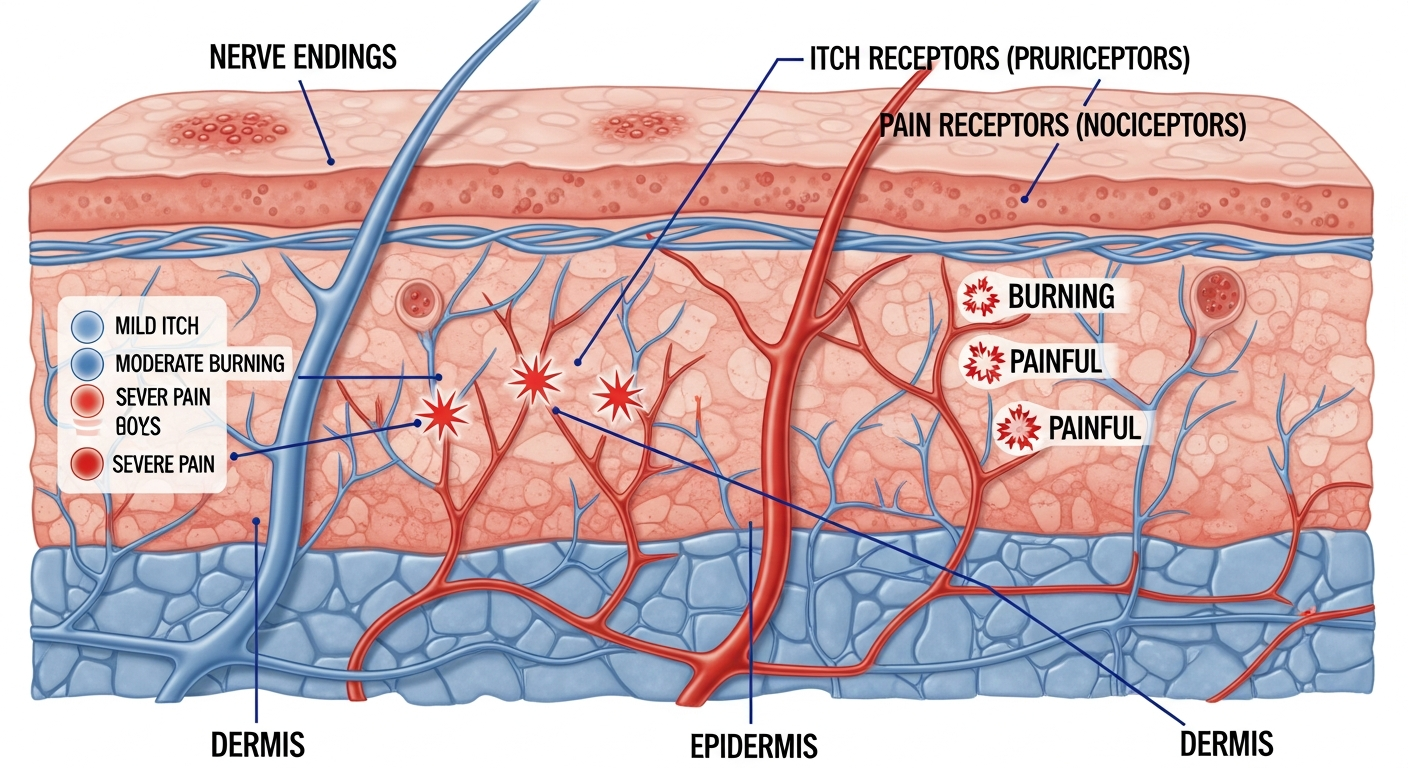
Leg rashes have a uniquely broad diagnostic spectrum — from the benign (folliculitis from shaving) to the medically significant (venous eczema heralding chronic venous insufficiency) to the genuinely dangerous (cellulitis from bacterial skin infection). The precise location on the leg is a primary diagnostic clue: venous eczema and stasis dermatitis concentrate on the lower leg and medial (inner) ankle; atopic eczema flares behind the knees (popliteal fossae); erythema nodosum causes painful deep nodules on the front of the shins; lichen planus characteristically affects the ankles; and contact dermatitis from elastic socks or rubber boots creates a band exactly matching the elastic or boot-top contact area. Understanding these anatomical patterns is essential for accurate self-assessment before a medical consultation. This comprehensive guide covers the most important leg rash causes by location, their distinguishing features, red flag warning signs, and evidence-based treatment — with internal links to our diagnosis guide, rash symptoms guide, and rash pictures gallery for visual comparison.
Quick Medical Summary
Most Common Causes of Leg Rash by Location
Lower leg and ankle: venous (stasis) eczema is the most common diagnosis in adults over 50 with varicose veins or venous insufficiency. Chronically elevated venous pressure causes fluid, protein, and red blood cells to leak into the surrounding skin, producing redness, scaling, and itching, with progressive hemosiderin staining — a rust-brown discoloration from hemoglobin breakdown products. Without compression therapy to address the underlying venous insufficiency, the skin can progress to lipodermatosclerosis (hardening) and venous ulcers. Cellulitis on the lower leg — a bacterial skin infection — produces a single expanding area of redness, warmth, swelling, and tenderness from an entry point (a cut, crack between toes from athlete's foot, or insect bite). It requires antibiotic treatment and monitoring for spreading. Behind the knees (popliteal fossae): atopic eczema in children and young adults — symmetric, intensely itchy, scaly, lichenified skin in both knee creases is virtually diagnostic of atopic eczema. Shins (front of lower legs): erythema nodosum — tender, deep-red to violet nodules (not surface patches) sitting in the fat layer beneath the skin — represents a reactive condition from an underlying trigger (streptococcal infection, IBD, sarcoidosis, pregnancy, drugs). Knees: psoriasis (thick, silvery, well-defined plaques on the extensor surface — outer knee) and the 'knees and elbows' distribution is classic. Ankles and lower legs: lichen planus (shiny, flat-topped, purple papules with Wickham's striae on the surface) and gravitational purpura in the elderly (fragile capillaries producing non-blanching red-brown spots).
Identifying Your Leg Rash: Key Distinguishing Features
Color is highly diagnostic for leg rashes. Bright red, warm, and expanding from a wound or skin break: cellulitis or erysipelas (bacterial). Rust-brown, scaling, around the medial ankle: venous eczema with hemosiderin staining. Purple, non-blanching: vasculitis, gravitational purpura, or (if accompanied by fever) meningococcal purpura. Deep red to violet, tender nodules on shins: erythema nodosum. Shiny purple, flat-topped papules on ankles: lichen planus. Well-defined, silver-scaled plaques on knees: psoriasis. Ring-shaped, scaly with advancing border: ringworm. The blanching test is essential for lower leg rashes: press firmly on any red or purple spots — blanching (turning white) indicates blood vessel dilation (inflammatory); non-blanching indicates blood outside vessels (purpura, vasculitis, meningococcal — seek urgent medical care). Texture differentiates: rough, scaly surface = eczema, psoriasis, ringworm, or venous eczema; smooth, raised = urticaria (hives); firm, deeper = erythema nodosum or cellulitis; blistered = allergic contact dermatitis, herpes zoster on a leg dermatomal band. Symmetry: venous eczema may affect both legs but is often worse on the dominant-use leg; eczema and psoriasis tend to be bilateral; cellulitis, ringworm, and erythema nodosum may be unilateral.
When to Worry: Red Flags for Leg Rash
The following features in a leg rash warrant urgent or emergency medical evaluation. Rapidly expanding redness, warmth, and swelling from a skin break with fever: cellulitis progressing toward septicemia — mark the border and see a doctor today; go to the ER if expanding despite antibiotics or if red streaking appears. Non-blanching purple spots on the legs: apply the glass test immediately — non-blanching spots may indicate meningococcal septicemia (life-threatening bacterial infection), vasculitis, or platelet dysfunction — seek emergency care unless cause is known (e.g., established gravitational purpura in the elderly). Painful, deep, expanding redness between the toes or on the lower leg with extremely disproportionate pain, crepitus (crackling sensation under the skin), and systemic toxicity: possible necrotizing fasciitis — a surgical emergency. Tender deep nodules on the shins (erythema nodosum) without an identified trigger such as a recent strep throat: requires systemic investigation including chest X-ray (sarcoidosis, tuberculosis), inflammatory bowel disease workup, and throat swab. Leg rash accompanied by joint swelling, pain, or stiffness may indicate psoriatic arthritis, reactive arthritis, or rheumatic disease — refer to rheumatology. Chronic non-healing ulcers surrounded by venous eczema indicate advanced venous disease requiring compression therapy, wound care, and sometimes surgical intervention.
Treatment Overview for Leg Rash
Venous eczema treatment is dominated by compression: graduated compression stockings (class 2, 23–32 mmHg) are the single most important intervention, addressing the underlying venous hypertension that drives all the skin changes. Without compression, topical treatments provide only partial relief. Apply topical corticosteroids (mild to moderate) for the inflammatory eczematous component, and emollients daily. Refer to vascular surgery if venous ulcers develop. Cellulitis requires oral antibiotics (flucloxacillin or cephalexin for typical Staph/Strep) for 7–14 days; IV antibiotics in hospital for rapidly spreading cellulitis, high fever, or failure to respond to oral treatment in 48 hours. Mark the border at presentation to monitor progression. Atopic eczema behind the knees: potent topical corticosteroids (mometasone furoate) for flares, daily emollient maintenance, and nighttime cotton pajamas to reduce scratching damage. Erythema nodosum: treat the underlying cause (e.g., antibiotics for streptococcal infection); NSAIDs (naproxen, ibuprofen) and rest with leg elevation for pain; prednisolone for severe cases. Psoriasis on the knees: potent or very potent topical steroids (betamethasone + calcipotriol combination) under occlusion for thick plaques, coal tar preparations, and systemic agents (methotrexate, biologics) for extensive disease. Ringworm: topical clotrimazole or terbinafine twice daily for 4 weeks. Contact dermatitis (elastic/rubber): identify and remove the specific allergen (patch testing); replace elastic socks with non-rubber-banded alternatives; topical steroid to clear the reaction.
Key Symptoms
- Rust-brown, scaling, itchy rash around inner ankle (venous eczema)
- Expanding warm, red, swollen area from a skin break on the lower leg (cellulitis)
- Symmetric intensely itchy, lichenified rash behind both knees (atopic eczema)
- Tender deep-red nodules on the front of the shins (erythema nodosum)
- Thick silvery plaques on the outer knees (psoriasis)
- Purple, flat-topped shiny papules on the ankles (lichen planus)
- Ring-shaped scaly rash anywhere on the leg (ringworm)
- Band-shaped rash matching boot top or sock elastic (contact dermatitis)
Treatment Options
- Venous eczema: compression stockings (class 2) — most important; topical steroid; emollient
- Cellulitis: flucloxacillin or cephalexin; IV antibiotics if severe or spreading
- Atopic eczema: potent topical steroid; daily emollient; trigger avoidance
- Erythema nodosum: NSAIDs; treat underlying cause; leg elevation; rest
- Psoriasis: betamethasone + calcipotriol; biologics for severe disease
- Ringworm: topical antifungal for full 4 weeks
- Contact dermatitis: patch test; remove allergen; topical steroid
- Gravitational purpura: compression stockings; reassurance (benign in elderly)
| Condition | Typical Leg Location | Appearance | Urgent? |
|---|---|---|---|
| Venous Eczema | Medial ankle, lower leg | Rust-brown scale, itchy, hemosiderin | No — chronic management |
| Cellulitis | Any, from entry point | Red, warm, expanding, tender | Yes — antibiotics today |
| Atopic Eczema | Behind knees, symmetric | Lichenified, intensely itchy | No — flare management |
| Erythema Nodosum | Front of shins | Deep tender red nodules | Workup needed — systemic cause |
| Psoriasis | Outer knees, extensor | Thick silver plaques, sharp border | No — chronic management |
| Meningococcal Purpura | Any, rapidly spreading | Non-blanching purple spots + fever | Emergency — call 999/911 |
Diagnose and Treat Your Rash
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.