Rash on Hands: Causes, Diagnosis, and Treatment
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
March 18, 2026
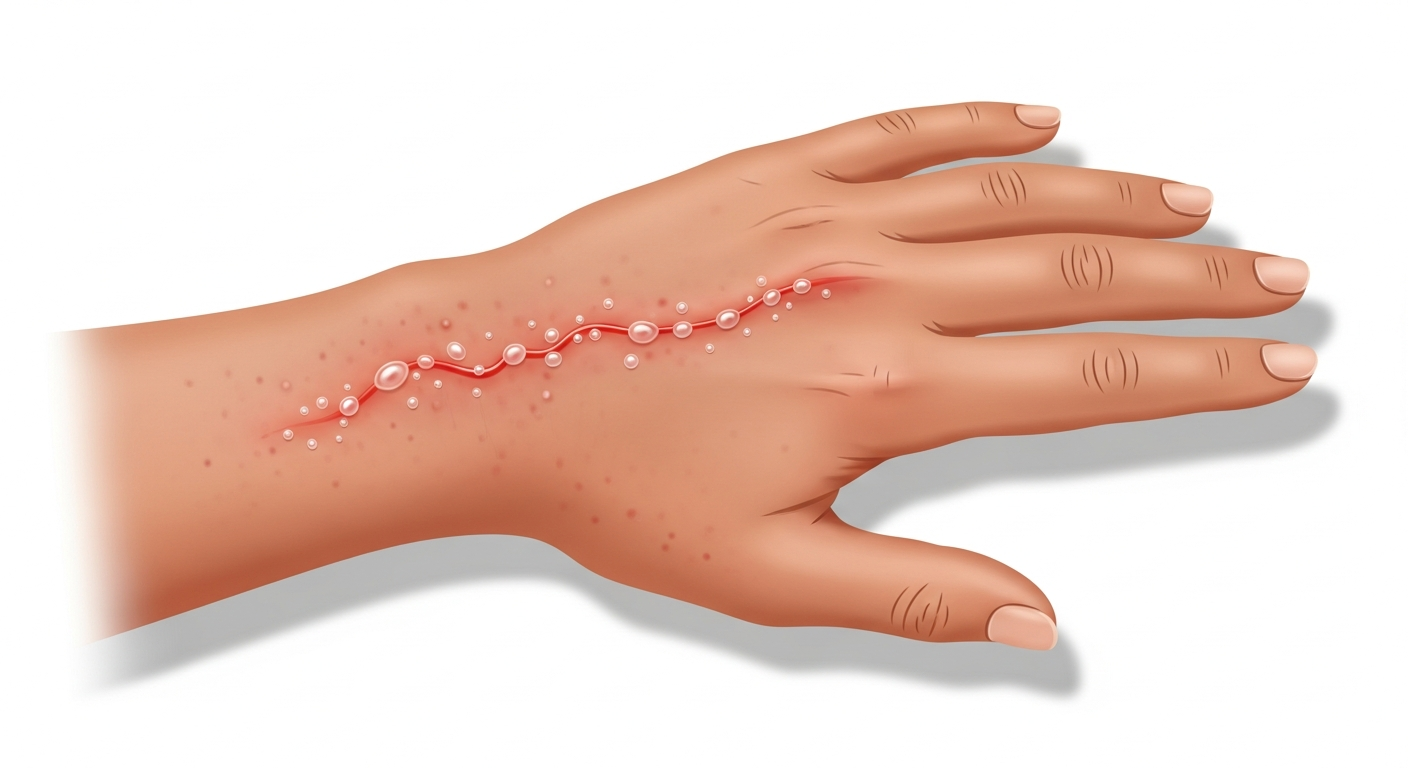
Hand rashes are among the most common dermatological presentations worldwide, and the hands have extraordinary exposure to potential triggers: soaps, detergents, cleaning chemicals, food, metals, rubber, and environmental allergens — often many times per day. The hands are simultaneously a primary site for both the most common rash type (irritant contact dermatitis from wet work) and among the most diagnostically challenging (dyshidrotic eczema, tinea manuum, and palmoplantar psoriasis can all appear similar). The key diagnostic principles for hand rash are: (1) identify whether both hands are equally affected (bilateral: eczema, psoriasis) or predominantly one hand (unilateral: tinea manuum — the 'two feet one hand' syndrome); (2) note the precise location (dorsum — back of hand — vs. palms vs. finger webs vs. fingertips); (3) determine whether blisters are present (dyshidrotic eczema, allergic contact dermatitis) or whether scaling predominates (psoriasis, irritant dermatitis, tinea); (4) assess occupational history — wet-work occupations (healthcare, food service, hairdressing, cleaning) cause the majority of occupational hand dermatitis. This guide covers all major hand rash causes with a comparison table and treatment protocols.
Quick Medical Summary
Most Common Causes of Hand Rash
Irritant contact dermatitis (ICD) is the most prevalent cause of hand rash globally. It results from repeated exposure to water, soaps, detergents, disinfectants, and solvents that strip the skin's lipid barrier, causing dryness, redness, cracking, and fissuring — predominantly on the fingertips and the dorsum of the hands. Healthcare workers, food handlers, hairdressers, and cleaners are disproportionately affected. The skin looks windburned or severely chapped. Allergic contact dermatitis (ACD) requires prior sensitization and produces a more intensely inflammatory reaction — blistering, weeping, and intense itch at the exact site of allergen contact. Common hand allergens include nickel (costume jewelry clasps, belt buckles), rubber accelerators in latex or vinyl gloves, fragrances and preservatives in hand creams and soaps (methylisothiazolinone, parabens), acrylates in nail products, and occupational chemicals. Dyshidrotic eczema (pompholyx) produces tiny, deep-seated vesicles (blisters) along the lateral sides of the fingers and on the palms, with intense itch and burning. The blisters are 'tapioca-like' — small, clear, deep-seated, and do not rupture as readily as surface blisters. They dry and peel over 2–4 weeks, leaving cracked skin. Triggers include sweating, stress, nickel exposure, and atopy. Tinea manuum (ringworm of the hand) is notably underdiagnosed and is strongly suggested by unilateral hand involvement: the 'two feet, one hand' syndrome — scaly dermatitis of both feet and one hand, caused by autoinoculation of tinea pedis from feet to one dominant hand. The scaling is dry and powdery with a slightly raised border. Scabies involves the web spaces between fingers, wrists, and sides of hands with characteristic burrow lines and intense nocturnal itching.
Symptom Breakdown: Hand Rash by Location and Morphology
The location of the rash on the hand is highly diagnostically specific. Web spaces between fingers: scabies (thin burrow lines with intense night itch), contact dermatitis from rubber gloves (in the exact glove web coverage area). Fingertips and fingernail area: irritant contact dermatitis from excessive washing; paronychia (bacterial or candidal infection around the nail margin); contact dermatitis from acrylates in nail products; palmoplantar psoriasis (pustular form with sterile pustules). Palm (thenar and hypothenar eminences): dyshidrotic eczema, palmoplantar psoriasis (thick, scaly plaques that can crack and cause significant pain), tinea manuum (dry, scaling, usually one-sided). Dorsum (back of hand): irritant or allergic contact dermatitis from gloves, most commonly on the dorsal hand surface; ringworm (classic ring shape with scaly outer border). Ring fingers: nickel or gold allergy from rings — the rash is exactly ring-shaped, matching the ring contact. Hand eczema in the palmodigital distribution (palms + finger undersides) is often dyshidrotic eczema or atopic hand eczema. The morphology is crucial: blisters → dyshidrotic eczema or ACD; dry scaly cracking → ICD or tinea manuum; thick plaques → palmoplantar psoriasis; tiny pus-filled spots (pustules) at nail margin → psoriasis or bacterial paronychia.
When to Worry: Red Flags for Hand Rash
Most hand rashes, while uncomfortable and impairing hand function, are not dangerous. However, specific presentations warrant urgent evaluation. Rapidly spreading warmth, redness, and swelling from a small cut or puncture wound on the hand, with fever: hand or finger cellulitis — the hand's closed tendon sheaths can allow infection to track rapidly, causing serious damage if not treated promptly. See a doctor today or go to an emergency department. Paronychia (infection at the nail edge) that develops red streaking along the finger or dorsal hand: suggests spread along the tendon sheath — surgical drainage and antibiotics may be needed. Painful, intensely itchy blisters on the hand in a person who was working with chemicals, industrial solvents, or epoxy resins: severe irritant or allergic contact reaction requiring medical evaluation, removal from exposure, and possibly prescription treatment. Dominant-hand tinea manuum (unilateral hand rash) treated repeatedly with topical steroids that appears to improve but recurs: tinea incognito — the steroid suppresses the surface inflammation while the fungal infection spreads; stop steroids and start antifungal treatment. Scabies affecting the entire body (hand web spaces, wrists, axillae, genitalia, buttocks) in multiple household members simultaneously: treat all contacts simultaneously with permethrin 5% cream to prevent re-infestation cycle. Bleeding, non-healing, or keratotic lesions on sun-exposed hand skin in older adults: may represent actinic keratoses or squamous cell carcinoma requiring dermatological biopsy.
Treatment Overview for Hand Rash
Irritant contact dermatitis treatment focuses on barrier protection and barrier repair: use a pH-balanced, fragrance-free hand cleanser rather than regular soap; apply a thick barrier cream (zinc oxide-containing or petrolatum-based) before tasks involving water or chemical exposure; wear vinyl (not rubber) gloves for wet work; apply rich emollient immediately after each handwash while hands are still damp. Prescription topical steroids (betamethasone valerate 0.1% or mometasone furoate 0.1%) clear acute flares rapidly. Allergic contact dermatitis requires allergen identification via patch testing and permanent avoidance of the specific allergen — without allergen elimination, the rash returns regardless of treatment. Dyshidrotic eczema: mid-to-high potency topical steroids during the active vesicle phase; emollients during the peeling/resolution phase; nickel avoidance (dietary and contact); stress management. For refractory dyshidrotic eczema, dupilumab (biologic) is increasingly used and highly effective. Alitretinoin (oral retinoid) is approved specifically for chronic hand eczema refractory to topical steroids in several countries. Tinea manuum: topical terbinafine 1% cream twice daily for 6 weeks on the hand; simultaneously treat tinea pedis (athlete's foot) with the same agent on both feet — failing to treat the feet guarantees rapid reinfection of the hand. Palmoplantar psoriasis: very potent topical steroids (clobetasol 0.05%) under occlusion (saranwrap overnight); acitretin (oral retinoid) is particularly effective for palmoplantar pustular psoriasis; biologics for severe disease.
Key Symptoms
- Dry, red, chapped, fissured skin on fingertips and dorsal hand (irritant dermatitis)
- Intensely itchy deep vesicles along finger sides and on palms (dyshidrotic eczema)
- Thick, cracked, scaly plaques on palms (palmoplantar psoriasis)
- One-sided scaly hand rash with both feet affected (tinea manuum)
- Burrow lines in web spaces with severe night itch (scabies)
- Ring-shaped rash under finger ring (nickel allergy contact dermatitis)
- Pustules or pus at nail edge (bacterial paronychia or pustular psoriasis)
- Blistering rash in exact glove contact pattern (allergic contact dermatitis)
Treatment Options
- ICD: barrier cream + vinyl gloves + gentle cleanser; topical steroid for flares
- ACD: patch test to identify allergen; strict permanent allergen avoidance
- Dyshidrotic eczema: potent topical steroid; emollients; nickel avoidance; dupilumab
- Tinea manuum: terbinafine cream 6 weeks; simultaneously treat both feet
- Palmoplantar psoriasis: clobetasol under occlusion; acitretin; biologics
- Scabies: permethrin 5% cream full body; treat all household contacts same day
- Hand paronychia: warm soaks; antibiotics; surgical drainage if abscess
- Occupational hand dermatitis: workplace assessment; modified duties; emollient regimen
| Condition | Predominantly One or Both Hands? | Blisters? | Primary Location |
|---|---|---|---|
| Irritant Contact Dermatitis | Both | No — dryness/cracking | Fingertips, dorsum |
| Dyshidrotic Eczema | Both (sometimes one worse) | Yes — deep-seated vesicles | Finger sides, palms |
| Tinea Manuum | One hand (dominant) | No — fine scaling | Palm, extending to dorsum |
| Palmoplantar Psoriasis | Both | Sterile pustules (pustular type) | Palms and soles |
| Allergic Contact Dermatitis | Matches contact shape | Yes — weeping blisters | Glove coverage area or ring area |
| Scabies | Both wrists and web spaces | No — burrow lines, papules | Finger webs, wrists, sides of hands |
Diagnose and Treat Your Rash
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.