Rash on Face: Causes, Symptoms, and Treatment
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
February 14, 2026
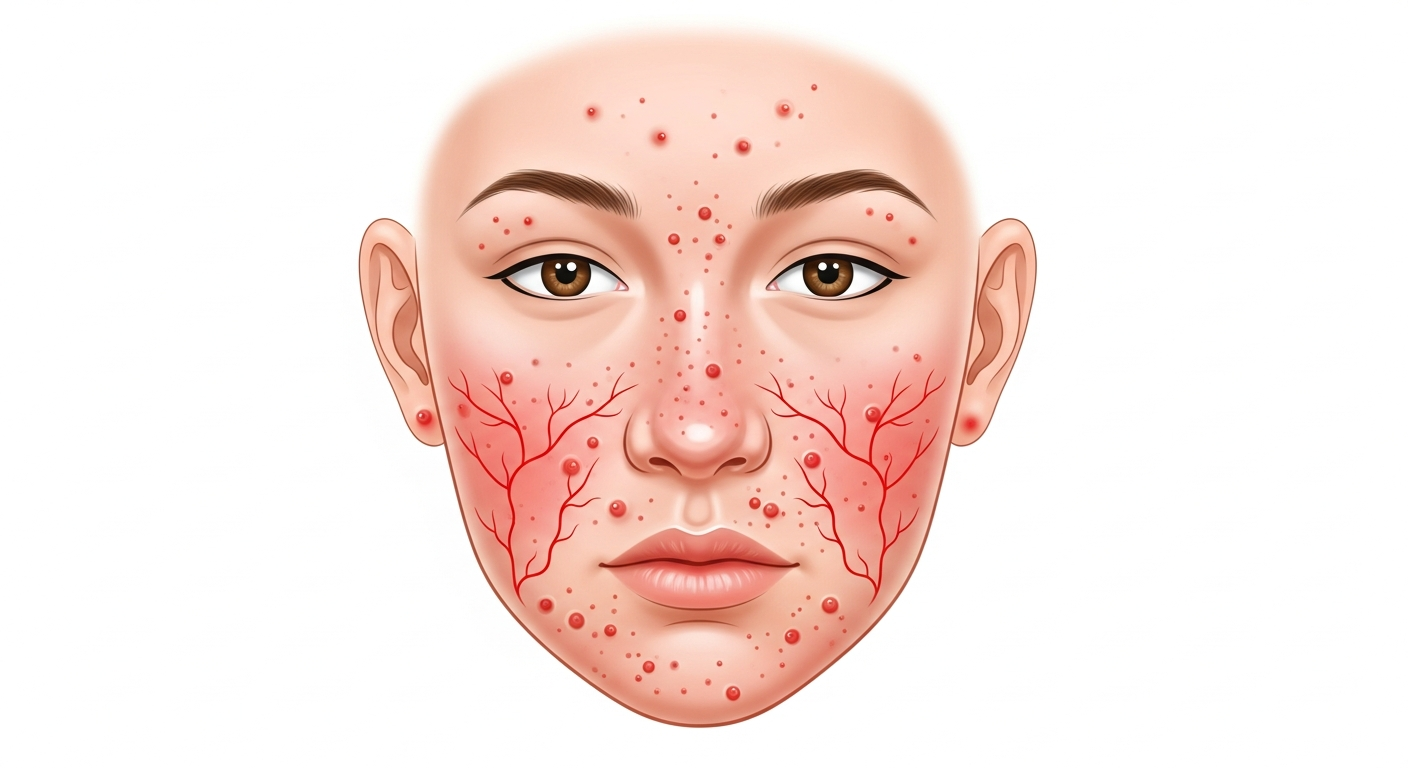
A rash on the face is one of the most distressing dermatological presentations because it is constantly visible and can significantly impact confidence, social interaction, and quality of life. The face has unique skin properties that predispose it to specific conditions: higher sebaceous gland density on the central face (nose, forehead, chin) promotes conditions like rosacea, seborrheic dermatitis, and acne; the thin, sensitive periorbital and perioral skin reacts readily to allergens in cosmetics and topical treatments; and the face is perpetually sun-exposed, predisposing it to photodermatoses and UV-triggered autoimmune flares. The eight most important facial rash diagnoses are rosacea, seborrheic dermatitis, contact dermatitis (from cosmetics, sunscreen, or metals), perioral dermatitis, atopic eczema, the malar rash of lupus erythematosus, impetigo, and herpes simplex labialis. Each has a distinct morphology, distribution, and treatment approach — accurate diagnosis is critical because the treatment for one (topical steroids for eczema) can dramatically worsen another (rosacea, ringworm, perioral dermatitis). This medically reviewed guide walks through the major causes, their identifying features, and evidence-based treatment for each. Use the comparison table below and links to our specialist silo pages to navigate the diagnosis most relevant to your situation.
Quick Medical Summary
Most Common Causes of Facial Rash
Rosacea is the leading cause of chronic facial redness in adults over 30, affecting the central face — cheeks, nose, chin, and forehead — with persistent redness, visible blood vessels (telangiectasia), flushing triggered by heat/alcohol/spicy food, and in papulopustular rosacea, red papules and pustules resembling acne without comedones (no blackheads or whiteheads). Seborrheic dermatitis targets oily skin areas: the nasolabial folds (beside the nose), eyebrows, ear canal rims, and hairline, producing yellowish-white, greasy scale on a red base — caused by an inflammatory response to Malassezia yeast. Perioral dermatitis produces clustered small papules and pustules specifically around the mouth, often sparing a 2–3mm zone adjacent to the lip border — it is strongly associated with prolonged topical steroid use, inhaled steroids, and certain dental products. Contact dermatitis from cosmetics, fragrances, sunscreen chemicals, nickel (in eyeglass frames), or hair dye (PPD) produces a rash in the shape and distribution of the allergen contact — a band across the forehead from a hair dye reaction, bilateral redness from a fragrance in moisturiser, or redness at the nose bridge from nickel eyeglass frames. Atopic eczema (in adults) most commonly involves the eyelids and periorbital skin — intensely itchy, scaly, thickened skin that typically reflects allergen contact (cosmetics, eye drops, contact lens solutions). Impetigo — a bacterial infection common in children — produces honey-colored crusted sores around the nose and mouth requiring antibiotic treatment. The malar (butterfly) rash of systemic lupus erythematosus spans both cheeks and the nose bridge in a fixed, photosensitive eruption that characteristically spares the nasolabial folds, distinguishing it from rosacea and seborrheic dermatitis.
Symptom Breakdown: Identifying Your Facial Rash
Location on the face is the single most diagnostically useful feature. Central face (cheeks and nose): rosacea, seborrheic dermatitis, lupus malar rash, and acne. Perioral only (around the mouth): perioral dermatitis. Eyelids and periorbital: atopic eczema, contact dermatitis from eye products. Nose creases and eyebrows: seborrheic dermatitis. Forehead hairline: seborrheic dermatitis, contact dermatitis from hair products. Ears: seborrheic dermatitis, contact dermatitis, discoid lupus. Morphology distinguishes rosacea from acne: rosacea has no comedones (blackheads/whiteheads) whereas acne has multiple; rosacea is triggered by heat/alcohol and causes background persistent redness rather than individual lesions resolving independently. Scale distinguishes seborrheic dermatitis (yellowish-greasy) from eczema (white-fine) from psoriasis (thick-silver). Photosensitivity distinguishes lupus (worsens in sun), photocontact dermatitis (confined to sun-exposed areas), and polymorphic light eruption (décolletage and outer face) from conditions that are sun-neutral. Timing helps too: rosacea and seborrheic dermatitis are chronic with flares; herpes simplex recurs in the same lip-border location with prodromal tingling; hives from facial allergens appear within 30 minutes and resolve within 24 hours. The blanching test applies to facial rashes: any non-blanching facial rash is a red flag for meningococcal disease or vasculitis.
When to Worry: Red Flag Signs for Facial Rash
Most facial rashes are inflammatory and not dangerous, but specific warning features demand urgent evaluation. Non-blanching facial rash — particularly when accompanied by fever, neck stiffness, or severe headache — may indicate meningococcal septicemia, a life-threatening bacterial infection. Press a glass against the spots: if they remain visible, call emergency services immediately. Facial swelling, particularly of the lips, tongue, or periorbital tissue (angioedema) alongside a rash may indicate anaphylaxis — use an epinephrine auto-injector if available and call emergency services. Spreading redness, warmth, and tenderness on one side of the face, accompanied by fever, may indicate facial cellulitis or erysipelas — a bacterial infection requiring antibiotics. Unilateral blistering rash on the face following the distribution of the trigeminal nerve (one cheek, one side of forehead, or one side of nose) with burning pain preceding the rash suggests herpes zoster ophthalmicus (shingles involving the eye) — a same-day ophthalmology emergency, as it can cause permanent vision loss if untreated within 72 hours. Butterfly rash accompanied by joint pain, fatigue, hair loss, and oral ulcers suggests systemic lupus erythematosus and warrants rheumatology referral with lupus serology (ANA, anti-dsDNA). Any new facial rash after starting a medication — particularly the antibiotics minocycline and doxycycline, sulfonamides, or antifungals — may be a drug reaction requiring medical evaluation.
Treatment Overview for Facial Rash
Treatment is diagnosis-specific. For rosacea: azelaic acid 15% gel (first-line for papulopustular), topical metronidazole 0.75–1% gel (anti-inflammatory), topical ivermectin 1% cream (for the Demodex mite component), brimonidine or oxymetazoline gel for erythema/flushing, oral doxycycline 40mg (modified-release) for moderate-to-severe papulopustular, and laser/IPL for telangiectasia. For seborrheic dermatitis: ketoconazole 2% cream applied twice daily for 2–4 weeks and maintained weekly, selenium sulfide or pyrithione zinc antifungal shampoo used as a face wash, or ciclopirox cream. For perioral dermatitis: stop all topical steroids (expect initial worsening — 'steroid rebound'), apply topical metronidazole 0.75% gel twice daily, and for severe cases, oral doxycycline 100mg twice daily for 6–12 weeks. For contact dermatitis: patch testing identifies the allergen; remove it; apply mild topical steroid (hydrocortisone 0.5–1% on the face for maximum 5–7 days); switch to fragrance-free, preservative-free cosmetics. Note: stronger steroids should not be used on the face. Tacrolimus 0.03% or pimecrolimus 1% are steroid-sparing options specifically approved for facial eczema. For lupus malar rash: hydroxychloroquine 200–400mg daily (reduces flare frequency and protects organs), strict sun protection (SPF 50+ broad-spectrum daily, UV-protective clothing and hats), and rheumatology co-management. For herpes simplex: topical aciclovir 5% cream or oral valaciclovir 500mg twice daily at the prodrome stage. For shingles (herpes zoster) on the face: oral valaciclovir 1g three times daily for 7 days, started within 72 hours of rash onset, and same-day ophthalmology if eye involvement is suspected.
Key Symptoms
- Persistent central-face redness with flushing triggers (rosacea)
- Yellowish-white scale in nose creases, eyebrows, or ears (seborrheic dermatitis)
- Perioral papules and pustules sparing the lip border (perioral dermatitis)
- Intensely itchy, scaly eyelid skin (contact/atopic eczema)
- Butterfly-shaped fixed red rash across cheeks and nose, photosensitive (lupus)
- Honey-colored crusted sores around nose or mouth (impetigo)
- Unilateral blistering with burning pain following nerve distribution (shingles)
- Non-blanching facial spots with fever and headache (emergency: meningococcal)
Treatment Options
- Rosacea: azelaic acid, topical metronidazole, oral doxycycline, laser for vessels
- Seborrheic dermatitis: ketoconazole 2% cream; antifungal shampoo as face wash
- Perioral dermatitis: stop steroids; topical metronidazole; oral doxycycline
- Contact dermatitis: remove allergen; patch test; mild hydrocortisone max 7 days
- Facial eczema: tacrolimus or pimecrolimus (steroid-free); fragrance-free moisturizer
- Lupus rash: hydroxychloroquine; strict SPF 50+ sun protection daily
- Impetigo: topical mupirocin or oral antibiotics
- Facial shingles: valaciclovir within 72 hours; ophthalmology same-day if eye involved
| Condition | Key Location | Hallmark Feature | Primary Treatment |
|---|---|---|---|
| Rosacea | Central face (cheeks, nose) | Persistent redness, no comedones, flushing | Azelaic acid, metronidazole, doxycycline |
| Seborrheic Dermatitis | Nasolabial folds, eyebrows, hairline | Yellowish-greasy scale | Ketoconazole 2% cream |
| Perioral Dermatitis | Around mouth, spares lip border | Clustered papules/pustules | Stop steroids; metronidazole |
| Allergic Contact Dermatitis | Matches allergen contact shape | Blistering, intense itch, delayed 24–72h | Remove allergen; mild steroid; patch test |
| Lupus Malar Rash | Butterfly: cheeks + nose bridge | Photosensitive, spares nasolabial folds | Hydroxychloroquine; sun protection |
| Facial Eczema | Eyelids, periorbital | Intensely itchy scaly skin | Tacrolimus; pimecrolimus; emollient |
Diagnose and Treat Your Rash
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.