Rash on Back: Causes, Identification, and Treatment
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
October 22, 2025
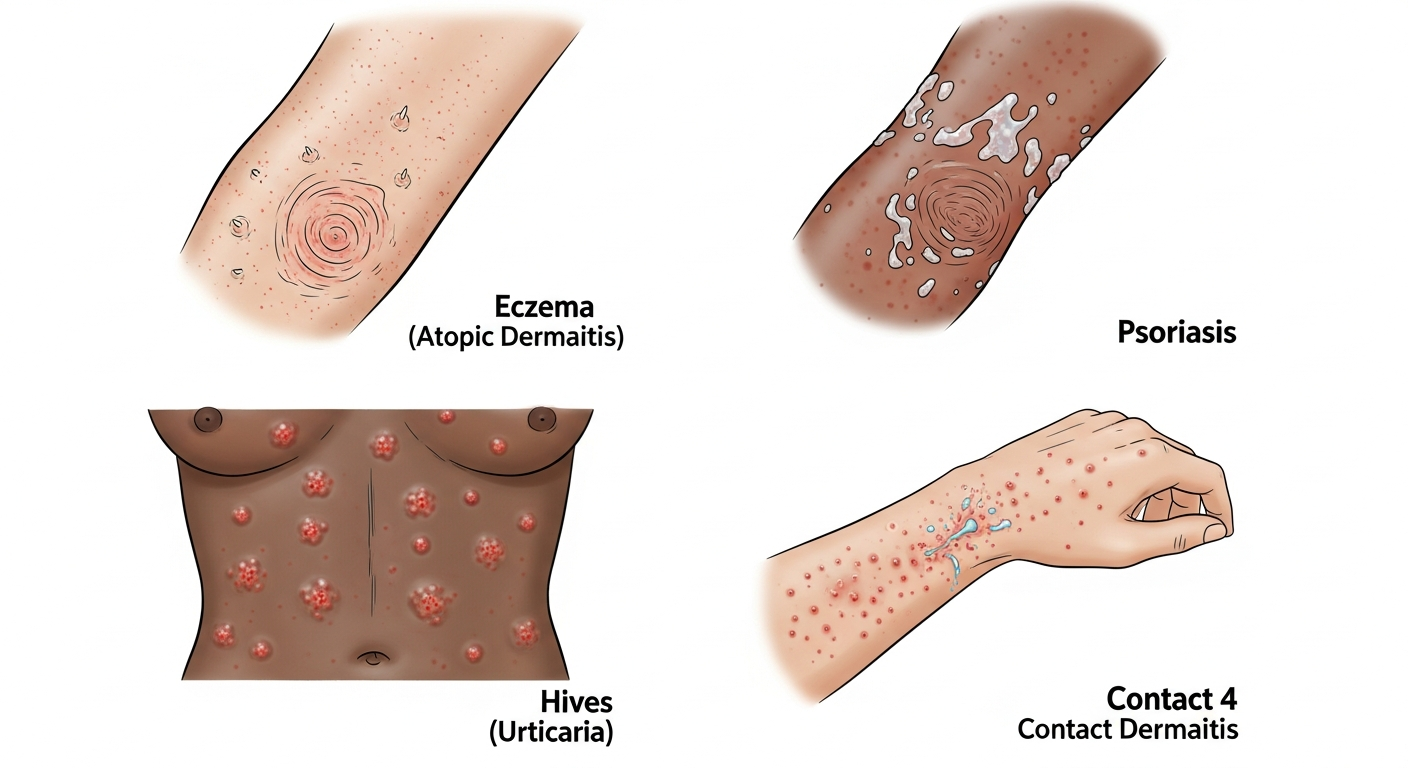
The back is one of the most common locations for a wide variety of skin rashes, partly due to its large surface area and partly because it is a frequently neglected area in daily skin care — rashes on the back are often discovered late because the patient cannot easily see them. The back has higher sebaceous gland density on the upper portion (shoulders, upper back) than the lower back, predisposing the upper back to acne vulgaris and tinea versicolor. It is also the most common location for pityriasis rosea's 'Christmas tree' pattern along Langer's lines, and a major site for atopic eczema in children who rub their backs against mattresses during sleep. Shingles on the back follows a dermatomal band from the posterior thorax around to the front chest on one side. Pressure-related rashes (from backpack straps, bra straps, or prolonged bed rest) cause friction contact dermatitis or pressure urticaria in specific strap-shaped patterns. This guide provides a comprehensive overview of back rash causes, diagnostic clues, and treatment approaches.
Quick Medical Summary
Most Common Causes of Back Rash
Acne vulgaris on the back (bacne) is extremely common in teenagers and young adults, driven by the high density of sebaceous glands on the upper back, friction from backpacks and bra straps, and occlusion from clothing and sports equipment. It presents as comedones (blackheads and whiteheads), papules, pustules, nodules, and cysts — often more severe and more inflammatory on the back than on the face. Truncal acne responds to the same treatments as facial acne but may require systemic treatment (oral antibiotics, isotretinoin) because topical application to the back is mechanically difficult. Tinea versicolor — Malassezia yeast overgrowth — produces multiple oval, hypo- or hyperpigmented patches on the upper back, chest, and shoulders. The patches fail to tan uniformly (appearing pale against tanned skin or slightly tan against untanned skin). The diagnosis is confirmed by Wood's lamp examination (copper-orange fluorescence) or KOH scraping (short pseudohyphae — 'spaghetti and meatballs' appearance). Pityriasis rosea distributes across the back in its characteristic Christmas-tree pattern — oval, salmon-colored patches oriented along the diagonally arranged Langer's lines of the back, producing a distinctive fir-tree silhouette. Psoriasis on the back produces well-defined, thick, silvery-scaled plaques, most commonly on the upper back and the lower sacral region (lumbosacral area). Sacral psoriasis is a particularly common and overlooked psoriasis location. Atopic eczema in children can affect the back when the child rubs their back against the mattress during sleep — an important and often overlooked sleeping-related trigger.
Symptom Breakdown: Back Rash by Appearance and Location
Upper back and shoulders: acne vulgaris (comedones, papules, pustules — follicular); tinea versicolor (multiple pale or tan oval patches, non-follicular); pityriasis rosea (oval patches in Christmas-tree pattern); psoriasis (thick silvery plaques). Mid-back: pityriasis rosea; viral exanthem (widespread, bilateral, beginning on trunk); drug rash (often starting on trunk). Lower back (sacral area): sacral psoriasis (particularly common — thick plaques on and above the gluteal cleft); lichen simplex chronicus (thickened, hyperpigmented skin from chronic scratching of an area the patient can reach — often the accessible lower back). Dermatomal band (any level of back): shingles — unilateral band from the posterior thorax curving around one side. Strap-shaped or banding pattern: contact dermatitis from bra straps (rubber elastic allergy), backpack straps, or seat-belt contact (seat belt dermatitis from neoprene or rubber). The presence of comedones (blackheads/whiteheads) distinguishes acne from all other back rashes — none of the other conditions produce comedones. The symmetry test: bilateral, symmetric = pityriasis rosea, psoriasis, acne, viral rash; strictly unilateral = shingles. The tanning test: are some patches paler than surrounding skin and fail to tan? This is tinea versicolor.
When to Worry: Red Flags for Back Rash
Most back rashes are benign but specific presentations require urgent evaluation. Unilateral back rash with severe burning pain that preceded the skin changes by 1–3 days: shingles. Begin antiviral therapy within 72 hours of rash onset to reduce severity and prevent post-herpetic neuralgia. Non-blanching rash on the back, particularly if accompanied by high fever, confusion, or neck stiffness: possible meningococcal septicemia — apply the glass test and call emergency services if spots remain visible under pressure. Rapidly spreading redness, warmth, and tenderness on the back from a wound, surgical scar, or skin break with fever: back cellulitis — requires antibiotics promptly; IV if rapidly expanding. Drug rash appearing on the back and spreading rapidly with systemic symptoms (fever, lymph node swelling, liver pain): DRESS syndrome or morbilliform drug eruption requiring medical evaluation. Non-healing, slowly enlarging dark or unusual lesion on the upper back (sun-exposed area): may represent melanoma or other skin cancer — sun damage accumulates on the upper back, which is a particularly high UV-exposure site. Any back lesion that changes in size, shape, color, or bleeds requires dermatological biopsy evaluation. Atopic eczema in a child severely affecting sleep due to back scratching on the mattress: this level of sleep disruption and excoriating behaviour warrants urgent dermatology referral for intensive treatment.
Treatment Overview for Back Rash
Back acne (bacne): daily cleansing with a benzoyl peroxide 5–10% body wash (leave on for 2–3 minutes before rinsing); topical retinoid (adapalene 0.1% gel) applied at night to non-irritated areas; topical clindamycin for bacterial component; oral doxycycline 100mg twice daily for moderate-to-severe inflammatory acne; isotretinoin for severe nodular or cystic back acne refractory to other treatments. Specific bacne triggers to address: change into dry clothing immediately after exercise; use oil-free, non-comedogenic sunscreen; carry a spare shirt if prone to sweating; avoid backpack pressure on active acne areas. Tinea versicolor on the back: selenium sulfide 2.5% shampoo applied to the back, left for 10–15 minutes, then rinsed off — three times weekly for 4 weeks; ketoconazole 2% shampoo as an alternative; a single oral dose of itraconazole 400mg or fluconazole 400mg if the infection is extensive. Note that pigmentary changes take 1–3 months to normalize after fungal clearance. Pityriasis rosea: self-limiting — treatment is symptomatic. Oral antihistamines for itch; calamine lotion; moderate sun exposure or narrowband UVB light accelerates resolution; oral aciclovir (800mg 5× daily for 1 week) may shorten the course based on recent evidence for HHV-7 trigger. Psoriasis on the back: potent topical steroids; calcipotriol; coal tar preparations; calcipotriol/betamethasone combination spray is particularly convenient for the difficult-to-apply back surface; phototherapy (UVB, PUVA); biologics for widespread or treatment-refractory disease. Back acne-related pigmentation: topical retinoids (adapalene, tretinoin) accelerate pigmentation resolution; azelaic acid; niacinamide 5–10% to reduce post-inflammatory hyperpigmentation.
Key Symptoms
- Comedones, papules, pustules, and nodules on upper back and shoulders (acne)
- Multiple pale or tan oval patches failing to tan uniformly (tinea versicolor)
- Oval salmon patches in Christmas-tree pattern along Langer's lines (pityriasis rosea)
- Thick silvery plaques on upper back or sacral area (psoriasis)
- Unilateral dermatomal band with burning pain (shingles)
- Strap-shaped rash matching bra strap or backpack strap (contact dermatitis)
- Itchy, lichenified patches in the reachable lower-back area (lichen simplex chronicus)
- Changing, dark, or non-healing lesion on sun-exposed upper back (seek dermatology)
Treatment Options
- Bacne: benzoyl peroxide wash; topical retinoid; oral doxycycline; isotretinoin for severe
- Tinea versicolor: selenium sulfide shampoo; oral itraconazole for extensive disease
- Pityriasis rosea: antihistamines; UVB; self-limiting (6–12 weeks)
- Psoriasis: calcipotriol/betamethasone spray; phototherapy; biologics
- Shingles: valaciclovir within 72h; gabapentin for post-herpetic neuralgia
- Contact dermatitis (straps): patch test; replace elastic/rubber straps; topical steroid
- Lichen simplex chronicus: potent topical steroid; habit reversal training; occlusion
- Suspicious lesion: dermatology biopsy — do not delay
| Condition | Back Location | Distinguishing Feature | Treatment Approach |
|---|---|---|---|
| Acne Vulgaris | Upper back, shoulders | Comedones (blackheads/whiteheads) present | Benzoyl peroxide; retinoid; oral antibiotics |
| Tinea Versicolor | Upper back, shoulders, chest | Pale or tan patches, fails to tan | Selenium sulfide shampoo; antifungals |
| Pityriasis Rosea | Entire back, mid and lower | Christmas-tree pattern along Langer's lines | Self-limiting; antihistamines; UVB |
| Psoriasis | Upper back, sacral area | Thick silver plaques, sharp borders | Potent steroids; phototherapy; biologics |
| Shingles | Any — one-sided band | Dermatomal band, pain-preceded blisters | Antiviral within 72 hours |
| Strap Contact Dermatitis | Bra strap / backpack area | Rash exactly matches strap shape | Patch test; allergen-free alternative straps |
Diagnose and Treat Your Rash
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.