Adult Rashes: Common Causes and Treatment for Ages 18–60
Medically Reviewed By
Dr. Marcus Chen, FAAD
Last Updated
December 10, 2025
Adult skin has fundamentally different characteristics from childhood skin — it is more exposed to occupational chemicals and allergens, it accumulates a lifetime of UV damage that modifies cellular behavior, and it reflects the cumulative burden of chronic inflammatory conditions that were first established in childhood but are now managed (or not) in the context of work, stress, alcohol, and medications. The major rash causes in adults ages 18–60 differ meaningfully from childhood: atopic eczema persists in about 30% of childhood cases and presents occupationally in wet-work professions; psoriasis peaks in incidence in young adults (ages 20–30) and again in older adults; rosacea is almost exclusively an adult condition; contact dermatitis from occupational and cosmetic allergens accumulates as sensitization develops with repeated exposure; urticaria becomes more likely to be chronic and idiopathic in adults than in children; and shingles (herpes zoster) risk begins to rise from the 30s onward in immunocompromised adults and climbs steeply from the 50s. This guide covers the characteristic adult rash presentations, occupational factors, psychosocial impact, and evidence-based treatment across the adult age range.
Quick Medical Summary
Most Common Adult Rashes and Their Characteristic Presentations
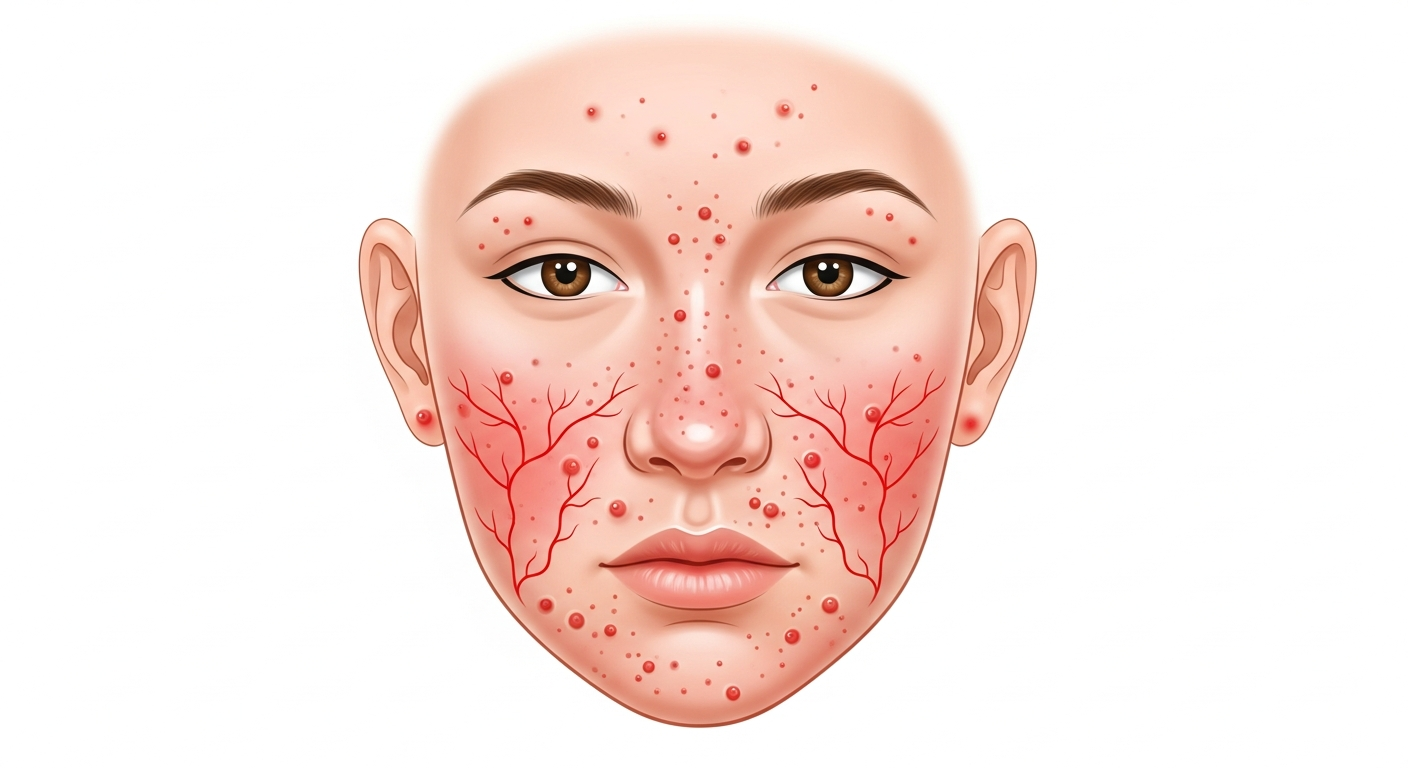
Rosacea is virtually exclusively an adult condition, typically beginning between ages 30 and 50, and predominantly affecting fair-skinned, Celtic or Northern European individuals. Women are affected three times more often than men, though men tend to develop the more severe phymatous (tissue thickening) subtype. Rosacea progresses through recognizable subtypes: erythematotelangiectatic (ETR — persistent facial redness and flushing with visible blood vessels); papulopustular (PPR — red papules and pustules resembling adult acne but without comedones, on the central face); phymatous (skin thickening, particularly rhinophyma — enlarged nose); and ocular rosacea (eye involvement, the most common subtype by patient prevalence). Psoriasis has a bimodal incidence — an early-onset type (ages 16–30) that tends to be more severe, more inflammatory, and associated with HLA-Cw6 genetic marker; and a late-onset type (ages 50–60) that tends to be more localized. Plaque psoriasis, the most common type (90% of cases), produces well-defined, thick, silver-scaled plaques on the elbows, knees, scalp, and lumbosacral area. Guttate psoriasis in younger adults is often triggered by streptococcal pharyngitis. Psoriatic arthritis (joint involvement) affects 30% of psoriasis patients and is an important co-morbidity requiring rheumatology co-management. Atopic eczema persisting into adulthood often concentrates on the hands, face, eyelids, and neck — areas with high allergen exposure. Hand eczema is particularly significant occupationally, as it can prevent people from performing their work effectively.
Contact Dermatitis, Urticaria, and Occupational Rashes
Contact dermatitis is disproportionately an adult disease because allergen sensitization requires repeated exposure over time — most people develop nickel allergy, fragrance allergy, or rubber chemical allergy in adulthood after years of cumulative exposure. Occupational contact dermatitis is a major cause of adult skin disease: hairdressers (hair dye PPD, bleach, rubber gloves), healthcare workers (latex, hand sanitizers, skin antiseptics), construction workers (cement chromate, epoxy resin, rubber), metalworkers (cutting fluids, nickel, chromate), and food workers (flour, garlic, spices) are all high-risk occupational groups. Occupational contact dermatitis has significant medico-legal implications and may qualify for workplace compensation, modified duties, or retraining. Chronic spontaneous urticaria (CSU) — hives occurring most days without an identifiable trigger for more than 6 weeks — is predominantly an adult condition. It affects approximately 1% of the adult population at any given time, more commonly women than men, with an average duration of 1–5 years. In 45% of CSU cases, autoimmune mechanisms are responsible (autoantibodies against the high-affinity IgE receptor on mast cells). Omalizumab (anti-IgE biologic monoclonal antibody) produces dramatic clearance in 60–70% of antihistamine-refractory CSU patients. Drug rashes are also more common in adults due to increasing medication use — NSAIDs, antibiotics, anticonvulsants, antihypertensives, and allopurinol are among the most common culprits. Adults on multiple medications have higher risk of drug-drug interactions that can enhance hypersensitivity reactions.
The Adult Immune System and Psychosocial Impact of Skin Rashes
The adult immune system from ages 18–60 represents peak immunocompetence in most respects — the best balance between innate and adaptive immunity, the most mature and educated T-cell and B-cell repertoire, and the most effective vaccine responses. However, specific vulnerabilities emerge. Pregnancy significantly alters immune function through progesterone-mediated Th2 skewing, predisposing pregnant women to conditions including obstetric cholestasis (severe itch), pemphigoid gestationis (autoimmune blistering rash), PUPPP (intensely itchy abdominal rash in late pregnancy), and exacerbation of existing eczema or rosacea. The postpartum period sees immune system rebound associated with flares of psoriasis and autoimmune conditions. HIV — increasingly managed in adulthood with antiretroviral therapy — is associated with a wide range of skin rashes including molluscum contagiosum, Kaposi's sarcoma, severe seborrheic dermatitis, and drug rashes from antiretroviral agents. Psychosocial impact of adult skin rashes is substantial: the visible nature of rashes, particularly on the face (rosacea, eczema) and hands (hand eczema), profoundly affects self-esteem, relationships, and employment. Studies consistently show that psoriasis, rosacea, and hand eczema patients have quality-of-life impairment comparable to that of patients with serious systemic diseases (cardiovascular disease, diabetes). Anxiety and depression are significantly more prevalent in adults with visible skin conditions. Referring adults with skin conditions to psychological support (CBT, psychodermatology services) alongside dermatological treatment improves both mental health and skin outcomes.
Prevention, Treatment, and When to See a Doctor for Adult Rashes
Prevention priorities for adults vary by condition. For rosacea: identify and avoid personal triggers (alcohol, hot drinks, spicy food, extreme temperatures, UV exposure); daily SPF 50+ broad-spectrum sunscreen; and gentle, fragrance-free skincare. For psoriasis: manage known triggers (stress, streptococcal infections, smoking, alcohol, certain medications including beta-blockers, lithium, and antimalarials). Smoking is a significant risk factor for psoriasis severity — smoking cessation improves both psoriasis and cardiovascular risk. For contact dermatitis: pre-task barrier cream, appropriate gloves (hypoallergenic vinyl rather than rubber for healthcare workers), fragrance-free products, and patch testing for identification of specific allergens. For shingles (from age 50+): the recombinant zoster vaccine (Shingrix) given in two doses provides 90%+ protection against shingles and post-herpetic neuralgia — it is recommended for all adults over 50. Seek urgent care for: non-blanching rash with systemic symptoms (meningococcal), blistering rash with mucosal involvement after starting a drug (SJS/TEN), throat swelling with hives (anaphylaxis). Seek same-day or next-day evaluation for: new drug-related rash that is spreading, cellulitis (expanding warmth and redness with fever), and shingles within 72 hours of rash onset (antiviral treatment must start promptly). Routine dermatology referral for: psoriasis affecting more than 10% body surface area or involving joints, chronic urticaria not responding to antihistamines, hand eczema preventing work, severe rosacea, or any changing skin lesion suspicious for skin cancer. For detailed diagnosis information, see how doctors diagnose skin rashes, and for visual rash identification, the rash pictures photo guide.
Key Symptoms
- Persistent central facial redness with flushing, no comedones (rosacea)
- Well-defined silvery plaques on elbows, knees, and scalp (plaque psoriasis)
- Dry, scaly, itchy hand rash in a wet-work occupation (occupational hand eczema)
- Hives persisting most days for >6 weeks without clear trigger (chronic urticaria)
- Contact-shaped rash from cosmetics, jewelry, or rubber gloves (contact dermatitis)
- Widespread pink rash 7–14 days after starting a new medication (drug rash)
- Unilateral blistering band with burning pain (shingles — urgent antiviral needed)
- Intense itch without rash in pregnancy (obstetric cholestasis — requires blood tests)
Treatment Options
- Rosacea: azelaic acid; metronidazole gel; doxycycline 40mg MR; laser for vessels
- Psoriasis: topical steroids + calcipotriol; phototherapy; methotrexate; biologics
- Occupational hand eczema: barrier cream + gloves; modify workplace; dupilumab
- Chronic urticaria: cetirizine (up to 4× dose); omalizumab for antihistamine-resistant
- Contact dermatitis: patch test; allergen avoidance; topical steroid; barrier cream
- Drug rash: stop suspected drug; assess for SJS if blistering; antihistamines
- Shingles: valaciclovir within 72h; neuropathic pain management
- Shingles prevention: Shingrix vaccine (2-dose course) from age 50
| Condition | Peak Adult Age Range | Key Feature | Treatment Cornerstone |
|---|---|---|---|
| Rosacea | 30–60, women > men | Central face flushing, no comedones | Trigger avoidance; azelaic acid; doxycycline |
| Plaque Psoriasis | 20–30 and 50–60 | Thick silvery plaques, elbows/knees | Topical steroids; phototherapy; biologics |
| Chronic Urticaria | 20–50, women > men | Daily hives >6 weeks, no clear trigger | Antihistamines; omalizumab |
| Occupational Dermatitis | 20–50 (working age) | Rash in occupational contact pattern | Patch test; allergen avoidance; workplace adjustment |
| Contact Dermatitis | Any adult age | Rash matches allergen contact shape | Allergen identification; permanent avoidance |
| Shingles (early risk) | 30s–60s (rising) | Unilateral dermatomal blistering + pain | Antiviral within 72h; Shingrix vaccine |
Further Reading by Age Group
When to See a Doctor Immediately
- Difficulty breathing or swallowing
- Swelling of the face, lips, or tongue
- High fever or severe chills
- Rapid spreading over a large body surface area
- Extreme pain, dizziness, or confusion
Frequently Asked Questions
Disclaimer
The medical information provided in this article is for educational purposes only and should not replace professional medical advice, diagnosis, or treatment. Always consult with a board-certified dermatologist or primary care physician regarding any severe or persistent skin conditions.